Who Should Use a CGM? A Guide to Benefits for Healthy Adults

Key Takeaways
- Who should use a CGM: Healthy adults use continuous glucose monitors to detect hidden glucose fluctuations and take preventative steps before metabolic issues develop.
- CGM lifestyle benefits: Tracking your individual glucose response provides 24/7 data that helps you build sustainable habits around diet, sleep, and exercise.
- Metabolic health monitoring: Pairing sensor data with Registered Dietitian guidance helps optimize your overall metabolic health rather than just managing existing conditions.
- Who should use a CGM: Healthy adults use continuous glucose monitors to detect hidden glucose fluctuations and take preventative steps before metabolic issues develop.
- CGM lifestyle benefits: Tracking your individual glucose response provides 24/7 data that helps you build sustainable habits around diet, sleep, and exercise.
- Metabolic health monitoring: Pairing sensor data with Registered Dietitian guidance helps optimize your overall metabolic health rather than just managing existing conditions.
Few would argue against the power of prevention when it comes to lowering the risk of chronic illness. Preventive medicine is often taken for granted, despite many devastating diseases having been successfully reduced or avoided through shifts in how we approach prevention.
But prevention is a moving target, especially as new advances in disease detection and preventive monitoring emerge–and this is where CGM devices have come into play. The technology behind continuous glucose monitors (CGMs) such as the Freestyle Libre 3 or Dexcom G7 isn't new. Even CGM devices themselves have been around since 1999, originally developed as a life-saving tool for diabetes management.
In this article, we’re stepping into the center of the conversation to address some of the biggest criticisms around the non-diabetic use of CGMs. We’ll explore the many sides of the argument and share evidence for why CGMs may be a helpful asset in wellness support.
How CGMs Benefit Healthy Adults

CGMs for healthy adults are a relatively new biohacking tool. If you don’t have prediabetes or diabetes, you may be skeptical about how CGM technology can benefit you and your health goals. But you might be surprised to learn that glucose levels in non-diabetics can fluctuate into pre-diabetic or diabetic range.
Understanding the factors that lead to dysregulated glucose levels can help you create healthier habits that can support stable energy levels, improve your sleep, and even support weight loss. Beyond this however, there’s also research showing that high glycemic variability is an independent risk factor for cardiovascular disease.
In addition to cardiovascular disease, higher glucose variability in non-diabetics has been associated with an increased risk of Alzheimer’s disease and cardiovascular death. According to Dr. Daniel Brito Guzmán, M.D, a cardiologist and assistant professor at the Heart and Vascular Institute at West Virginia University, healthy individuals can benefit from blood glucose monitoring by understanding how the pancreas and insulin work to maintain healthy blood sugar levels.
With this data and knowledge in hand, you can better understand what dietary and lifestyle habits may be contributing to your poor glycemic control.
What to Know About Glycemic Variability in Non-Diabetics
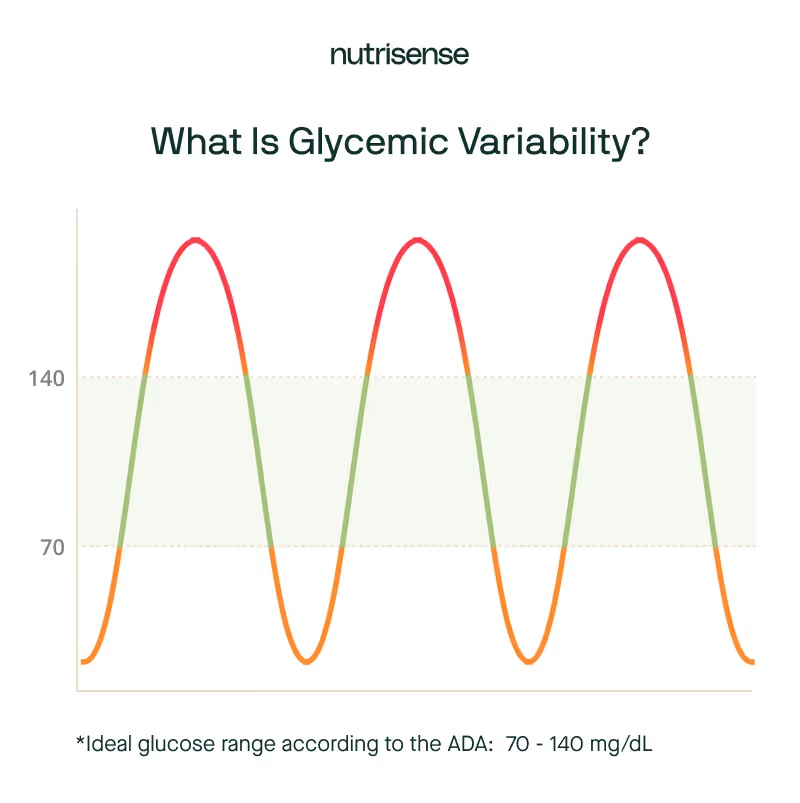
Glycemic variability is the degree to which your glucose fluctuates over time. And according to research, glycemic variability in non-diabetics is more common than you might think. One study conducted in 2018, for example, found that many individuals considered non diabetic by standard measures had high glucose variability revealed by the CGM. In fact, a quarter of the participants had severe glucose variability for up to 15 percent of the study duration, with glucose levels reaching the prediabetic range.
Another recent study reviewed the factors that contribute to postprandial hyperglycemia in non-diabetics. They found that post-meal glucose spikes of a certain quality are associated with greater hunger, poorer mental health and sleep as well as associated with greater mortality risk from cardiovascular disease.
However, these abnormalities in blood glucose stability (or dysglycemia) are usually only identified during a diabetes diagnosis through testing of hemoglobin A1C and/or fasting plasma glucose. Some research suggests that a CGM system may be a better indicator of pre-diabetes (early dysglycemia), than traditional types of glucose testing.
This is because glycemic variability is a uniquely important health metric that you can only assess with a CGM. A CGM is a tiny sensor that can enable real-time insight into glucose stability and insulin sensitivity and may encourage individuals and their health care providers to take early preventative steps for glucose management.
With this information in mind, let’s have a look at the many ways CGM technology can support metabolic health and healthy lifestyle habits and provide insight into the mechanics of your unique body.
1) CGMs for Metabolic Health

Most generally healthy people have likely never thought twice about their metabolic health, but it might surprise you that only 12 percent of Americans are actually metabolically healthy. That’s right—only one in eight American adults currently has optimal levels of things like HDL cholesterol, blood glucose, and blood pressure.
Uncontrolled blood glucose levels and insulin resistance are a risk factor for metabolic syndrome and diabetes mellitus. At the same time, controlled glucose levels can help reduce overstimulation of the pancreas and positively impact chronic inflammation.
There’s a great deal of unawareness among the general public when it comes to metabolic health, but CGMs are one tool that offers more insight into your blood sugar levels, which play a significant role in overall metabolic health.
According to Dr. Brito, understanding preprandial (pre-meal) and postprandial (post-meal) glucose levels can help people understand what dietary patterns lead to glucose dysregulation and use this information to create healthier habits.
2) CGMs for Healthy Lifestyle Changes

When it comes to diabetes, lifestyle modifications are proven to be the most effective intervention for normalizing fasting glucose levels and preventing diabetes among people with dysglycemia. For example, an early study published in the New England Journal of Medicine reported that lifestyle changes reduced the incidence of diabetes in those at high risk.
It showed that lifestyle changes reduced conversion to diabetes by 58 percent compared to a placebo, and by 39 percent over the drug metformin. But lifestyle changes can be hard to implement without guidance and accountability, which can make it challenging to stay on track.
In the CDC’s 2020 National Diabetes Statistic Report, authors noted that of the 84.1 million pre-diabetics living in the United States, only a shocking 11.6 percent were aware of their blood glucose problems.
Tools like CGMs that can provide real-time feedback on lifestyle factors, including diet, can be a low-risk accessible option for non-diabetics seeking to gain more awareness into their glucose readings and how they may be able to make choices that can impact their lifetime risk of disease.
Unpacking the Science Behind CGMs: Key Findings Revealed
CGMs do appear to have some clear benefits and health applications. However, some critics argue that there are no long-term randomized controlled clinical trials showing that people without diabetes benefit from tracking their glucose with CGMs.
And they’re right—there aren’t any yet. But, as physician and metabolic health expert Dr. Peter Attia points out in his article on CGMs:
“I can’t point you to a long-term randomized-controlled clinical trial rejecting the hypothesis that people with normal glucose responses don’t benefit from tracking their blood glucose because those trials don’t exist. There are examples where the randomized-controlled clinical trial data isn’t there, but we still have a strong reason to believe it’s true."
Other critics suggest that in people without diabetes, the body has an innate ability to maintain tight blood glucose regulation, so there’s no point in monitoring glucose data. However, a few recent studies reveal that glucose dysregulation such as hyperglycemia or hypoglycemia may be more common than once thought in this population.
For example, a 2021 study tracked the glucose levels of almost 500 people without diabetes using CGMs, and found glucose excursions into the diabetic range among 15 percent of healthy people. These findings suggest that CGM-guided personalized nutrition, which tailors food consumption to an individual's unique metabolic requirements and glycemic response, may in fact offer health benefits.
3) CGMs for Weight Loss and Weight Management
Another area of health where CGMs can potentially be useful is weight loss. Preliminary research from the Journal of Obesity Research and Clinical Practice suggests that continuous glucose monitoring is a well-tolerated and versatile tool for obesity research in pediatric and adult patients.
A recent review looked at 31 studies where CGMs were used to provide biofeedback, monitor dietary adherence, and assess glycemic variability in overweight and obese individuals. Overall, the researchers felt results were promising for obesity research. Study author and Pediatric Endocrinologist and Obesity Medicine Specialist Alaina P. Vidmar, MD, from the Kreck School of Medicine at the University of Southern California explained more in an interview with Nutrisense:
“We know that self-monitoring is very effective for some people. The association between what people are eating and how their body responds - seeing a visual of what their body is doing - helps them build a stronger association and helps them understand what is happening to their body.”
Dr. Vidmar went on to describe more about what she feels has been valuable in using CGMs in her research in non-diabetic youth:
“I’m all for the idea that the more tools we have, the more people we can help. What can we learn from CGMs in terms of prevention and intervention of obesity? Could we harness CGM data to help us? To have more understanding of what’s going on in the body? I think for people it can create a little bit more connection to their body and mindfulness.”
Obesity and early-stage type 2 diabetes are both associated with an increase in circulating insulin, a state known as hyperinsulinemia. Insulin is a hormone secreted by the pancreas to help regulate glucose homeostasis.
Research shows that hyperinsulinemia can precede and cause obesity and insulin resistance. In fact, in animal models, researchers have successfully demonstrated the causal role of hyperinsulinemia in obesity.
Unpacking the Science Behind CGMs: Key Findings Revealed

When it comes to using a CGM to help you lose weight, there are currently very few human studies available at this time. And this fact is what most critics will cite when dismissing the potential outright.
However, hyperinsulinemia and insulin resistance have proven links to obesity and weight gain. Several studies have shown that fasting hyperinsulinemia and insulin resistance in children and adolescents are risk factors for weight gain in later years.
A 2014 study published in the Indian Journal of Endocrinology and Metabolism suggested that the use of CGMS in the diagnosis of early prediabetes and insulin resistance, especially in high risk individuals, was promising. On many occasions, it was also found to be superior to other known diagnostic modalities, including oral glucose tolerance test (OGTT) and measurement of HbA1C.
At the end of the day, research affirms that there is no single best strategy for weight loss and weight management. Therefore, strategies should be individualized—and a CGM is capable of providing individualized data and feedback. A CGM sensor may be one tool among many used by qualified healthcare professionals to help you customize your dietary and lifestyle approach to fit your unique needs.
This sensor is not a weight loss device on its own, but when paired with expert metabolic health guidance from qualified nutritionists trained in assessing factors both related to glucose and beyond glucose, this holistic approach may help you uncover the most effective weight loss strategy.
{{rich-text-cta-wl2="/style-guide"}}
Interpreting CGM Data Correctly
At Nutrisense, we always recommend using a CGM with professional guidance to interpret your data and discuss how you can implement healthy lifestyle changes. The Nutrisense nutritionist team is made up of registered dietitians (RDs/RDNs) and certified nutrition specialists (CNS) with special training in metabolic health and a commitment to staying on top of the latest research.
They don’t just help you interpret your glucose data, they help you integrate multiple data points to create a customized approach to supporting your health goals. These data points include factors such as:
- Your symptoms
- Health history
- Deeper dietary analysis
- Laboratory biomarkers of metabolic health
Unpacking the Science Behind CGMs: Key Findings Revealed
With limited research identifying optimal glucose ranges in those without diabetes, critics ask: how can you know what glucose range to target? Although the research on normal glucose levels for non-diabetics is limited, it’s not completely absent.
Take for example, a 2019 study involving 153 healthy, non-diabetic participants who wore the latest generation CGM technology for an average of 192 hours. Below, you can see the insights that were revealed in this study.
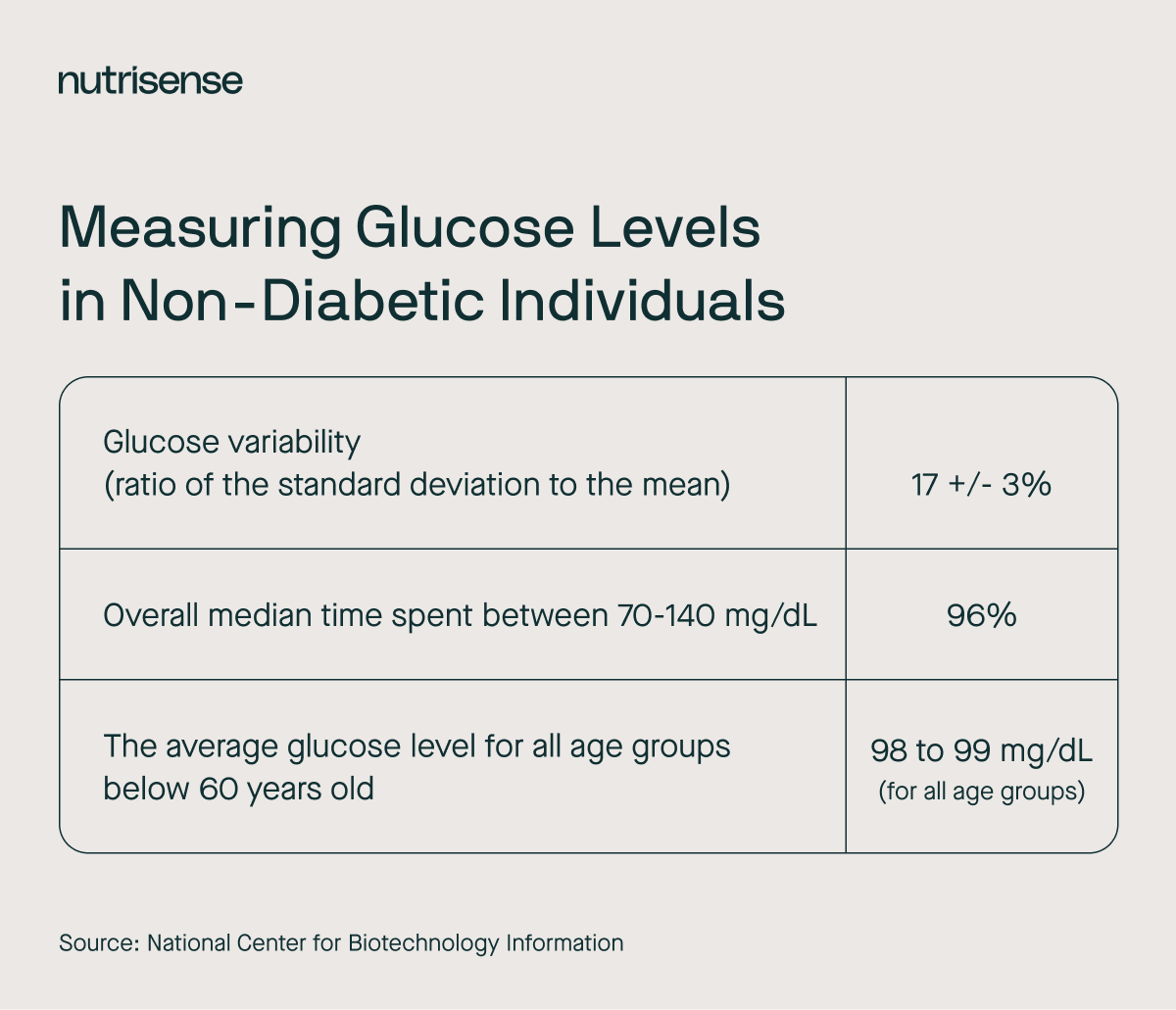

Researchers summarized, “Our study provides data for how often this target range and other ranges are achieved in individuals without diabetes. These data can be used as a benchmark for new diabetes technology and treatments.”
A more recent 2022 study used a “normal” range of 70–140 mg/dL to examine time in range for healthy individuals using CGMs. They concluded that the CGM may provide a better method of predicting the likelihood of individuals developing microvascular and macrovascular complications.
The American Diabetes Association further defines the ranges for normal glucose, prediabetes, and diabetes as shown here:

Nutrisense Members Share Their CGM Experiences
Here’s what a few Nutrisense members had to say about their experiences using the Nutrisense CGM and how the sensor has impacted their approach to healthy living.
Sara Duffy

“In the past five years, I had, in fact, gained 30, 35, maybe close to 40 pounds. Within the first month of using the CGM, I lost maybe five pounds. And I hadn’t been able to do that before. From February to June, I lost over 15 pounds! I noticed such a difference. And other people noticed, too, that I looked lighter and healthier. And it helped me refine my diet.”
Domenick Fraboni

"My biggest takeaway is that blood sugar is yet another amazing tool to help you have more information about your body. You can use it to better understand how to optimize sleep, exercise performance, recovery, mental clarity, and many other aspects of our everyday lives. I will definitely be revisiting the use of a CGM consistently.”
-Domenick Fraboni
Takeaways: How CGMs Can Support Better Well-Being
- CGM technology offers the ability to monitor, predict and motivate behavior change. Though research on the outcomes of using CGMs in non-diabetics is an emerging area with more work to be done, some studies already exist with promising potential.
- By partnering with an expert to help you combine CGM insights with deeper dietary analysis and other lab and symptom markers of metabolic health, a more meaningful interpretation of CGM data with experimental interventions may be possible.
- Nutrisense is not simply a CGM company and we don’t just focus on glucose. We are a metabolic health company that understands glucose regulation is one part of the larger picture of metabolic health. We believe in the power of prevention and personalization.
Find the right Nutrisense programto turn insight into progress.
Frequently Asked Questions
How does a CGM support a healthy lifestyle?
A CGM supports a healthy lifestyle by revealing your individual glucose response to food, sleep, and stress. This 24/7 data helps you move away from generic advice and build sustainable habits tailored to your unique metabolism.
How do you interpret CGM lab markers?
You interpret CGM lab markers by pairing 24/7 glucose data with expert guidance. A Registered Dietitian analyzes your individual glucose response alongside symptoms and health history to provide a complete picture of your metabolic health.
How do continuous glucose monitors improve metabolic health?
Continuous glucose monitors improve metabolic health by detecting early signs of glucose dysregulation. Tracking these fluctuations allows you to make targeted dietary and lifestyle adjustments before more serious metabolic issues develop.
Go Beyond Glucose Data with Nutrisense
Your glucose can significantly impact how your body feels and functions. That’s why stable levels are an important factor in supporting overall wellbeing. But viewing glucose isn't enough. Nutrisense, you’ll be able to learn how to use your body's data to make informed lifestyle choices that support healthy living.
One-to-one coaching
Sign up to access insurance-covered video calls to work with a glucose expert: a personal registered dietitian or certified nutritionist who will help tailor your lifestyle and diet to your goals.
Monitor and measure what matters
With the Nutrisense CGM Program, you can monitor your glucose with health tech like glucose biosensors and continuous glucose monitor (CGM)s, and analyze the trends over time with the Nutrisense App. This will help you make the most informed choices about the foods you consume and their impact on your health.
Find your best fit
Ready to take the first step? Start with our quiz to find the right Nutrisense program to help you take control.

Amanda is a Nutrition Manager and Registered Dietitian, with a Masters in Dietetics from Stephen F. Austin State University. Originally from south GA, she got her undergrad degree from Texas Tech University. She worked at a hospital in Fort Worth, TX, for 4 years as a dietitian, counseling those living with HIV.



.avif)
