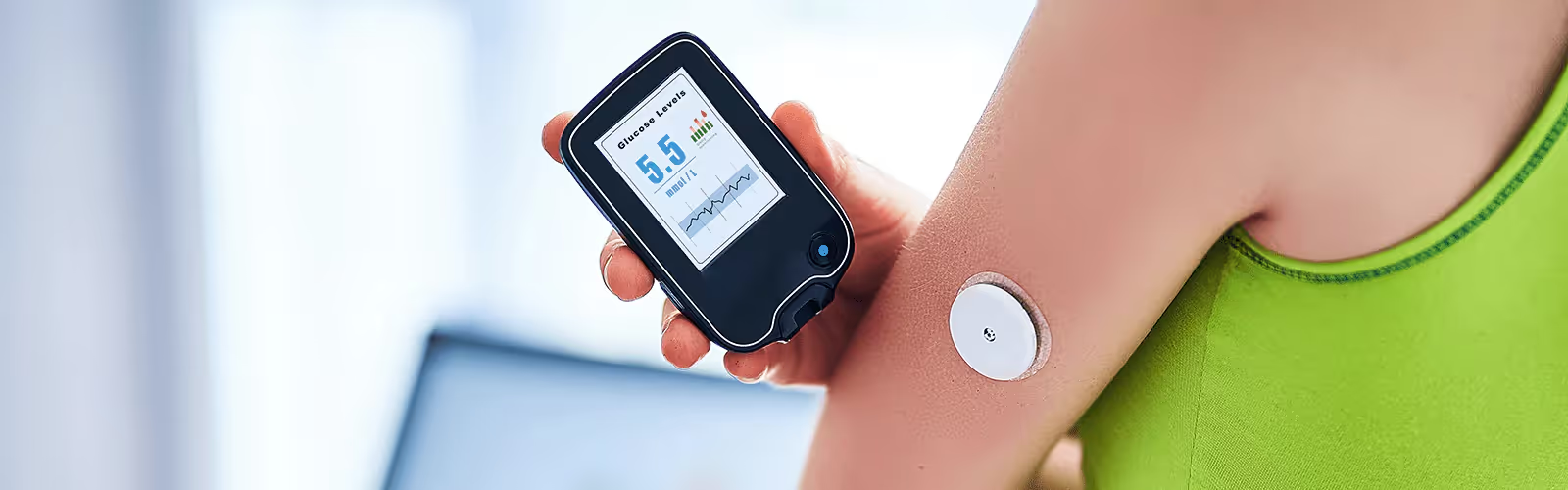
Difference Between Insulin and Glucagon: How They Work Together
Key Takeaways
- Insulin and glucagon functions: These two hormones work together to keep your glucose levels in an ideal range by constantly regulating the amount of glucose in your bloodstream.
- Difference between insulin and glucagon: Insulin lowers glucose values by helping cells absorb it for energy, while glucagon raises glucose by signaling the liver to release stored energy.
- Glucagon vs glucose: Glucose is the primary fuel your body uses for energy, whereas glucagon is the hormone that tells your liver to release that fuel.
- Insulin and glucagon functions: These two hormones work together to keep your glucose levels in an ideal range by constantly regulating the amount of glucose in your bloodstream.
- Difference between insulin and glucagon: Insulin lowers glucose values by helping cells absorb it for energy, while glucagon raises glucose by signaling the liver to release stored energy.
- Glucagon vs glucose: Glucose is the primary fuel your body uses for energy, whereas glucagon is the hormone that tells your liver to release that fuel.
If you really want to understand how to manage your blood sugar levels, you should get to know your hormone functions. Insulin and glucagon are essential building blocks of human biology. If you're monitoring your glucose levels for health and optimization reasons, it helps to know the nitty-gritty of the relationship these hormones have.
Our bodies work hard to continually keep our glucose in a tight range—only a few teaspoons are found in the bloodstream at any time. Insulin and Glucagon are the two hormones that work as opposing forces to constantly regulate glucose levels.
When insulin and glucagon are working in perfect harmony, our blood sugar levels will stay nice and balanced. But what happens if they are not in sync? Let’s take a look at how these two hormones keep your blood sugar within healthy limits.
What Are Insulin and Glucagon?

Insulin: An Anabolic Hormone
Hormones are chemical messengers. Their job is to carry instructions from one set of cells to another. For example, when certain situations occur (like eating a large carb-heavy meal), the beta cells in the pancreas instruct the release of insulin. Insulin is an anabolic hormone, meaning that it promotes growth. It has many functions, including lowering glucose values.
Insulin helps your cells take up glucose and use it as energy - or store it for future use. Without the messenger insulin, cells cannot use glucose as fuel, which can lead to them not working properly. If your body doesn’t make enough insulin, it can cause your blood sugar levels to rise.
Glucagon: A Catabolic Hormone
Glucagon is a hormone released from the alpha cells in the pancreas. Its chemical messenger effect is the opposite of insulin. Its primary function is to raise glucose levels if they get too low.
Glucagon is a catabolic hormone, meaning that it breaks down larger molecules. If blood sugar levels are low, glucagon tells your body to break down glycogen (stored glucose) in the liver to release glucose and increase glucose levels.
How Insulin and Glucagon Work Together
So, we’ve touched on the very basics. Insulin lowers your blood sugar levels, and glucagon raises them. They work opposite of each other, but also work together. However, there is a bit more to it than that.
How Insulin Works
Healthy individuals release insulin throughout the day in small quantities to constantly keep their glucose in that tight range mentioned earlier. But, when we eat (especially carbohydrates), we release a larger burst of insulin. After meals, your body goes into something called the ‘fed state’. In this state, insulin is at its highest, and you get your energy from the food you are eating.
Our digestive system breaks down the food we eat, and then the gut absorbs the glucose released from our food into the bloodstream -- raising blood sugar levels. This is when the hormones kick in. The rise in blood sugar stimulates the pancreas to release insulin. Insulin enables your body to take glucose out of the bloodstream into the cells so that they can use it for energy or store it for later.
Insulin has both upregulatory and deregulatory actions. Cells use upregulation to increase their sensitivity to a specific hormone. Deregulation means precisely the opposite and is when a cell makes itself less sensitive to a hormone.
Functions That Insulin Stimulates
- Glucose uptake from the bloodstream - the removal of glucose from the bloodstream to the cells
- Glycogen synthesis - the production of glycogen
- Lipogenesis - the formation of fatty acids
- Protein synthesis - the production of proteins
- DNA synthesis - the creation of DNA
- Gene expression - the conversion of DNA into a product, such as a protein
- Amino acid uptake - the taking in/use of amino acids
Functions That Insulin Inhibits
- Lipolysis - breaking down of fats
- Gluconeogenesis - the formation of glucose from a non-glucose source
- Apoptosis - programmed cell death
- Autophagy - the removal of damaged cells
How Insulin Controls Glucose Levels
Insulin is the key that allows your body to transport glucose and use it or store it as energy.
First, it allows your cells to use glucose for immediate energy. It pulls glucose out of your bloodstream and into your cells to convert it into adenosine triphosphate (ATP)—the cell’s primary energy currency.
If there is excess energy, insulin drives glucose into glycogen creation in the muscles and liver. In a healthy individual, 80-90% of consumed glucose gets stored as glycogen.
Insulin also suppresses gluconeogenesis to maintain lower glucose values.
How Glucagon Works
When blood sugar levels become low, your body signals the release of glucagon from the pancreas and primarily acts on the liver to raise glucose levels. Glucagon is usually released in a fasted state and during “fight or flight” moments. In these scenarios, glucagon tells your liver and muscle cells to break down stored glycogen back into glucose. The glucose is then released into your bloodstream so your cells can use it for energy.
How Glucagon Controls Glucose Levels
When glucose levels drop, glucagon acts on the liver to initiate gluconeogenesis and glycogenolysis.
Gluconeogenesis is the formation of glucose from a non-glucose source such as an amino acid, providing another source of glucose for the blood to raise blood sugar levels.
Glycogenolysis is the catabolic process of breaking down glycogen from the liver and muscle cells into glucose to produce more energy and raise blood sugar levels.
Acute stress also stimulates glucagon and inhibits insulin, causing glucose levels to increase.
As you can see, the relationship between insulin and glucagon is bidirectional. It keeps your blood sugar levels finely balanced while ensuring your body has a steady supply of energy. But, what happens if there is too much or too little of one of these hormones?
What Happens If You Have Too Much Insulin or Glucagon?
Understandably, this is one of the first questions people tend to ask when they start to learn about insulin and glucagon.
What Happens If I Have Too Much Insulin?

There are two critical outcomes from having too much insulin.
- Hyperinsulinemia is abnormally high levels of insulin in the blood. When insulin levels are high, your cells start to ignore the effects of insulin even though there is plenty of it available. This leads to insulin resistance.
- Insulin Resistance causes your cells to reject glucose. Glucose then remains in the bloodstream, elevating blood glucose levels, and the pancreas continues to produce more and more insulin.
Put simply—too much insulin in the blood leads to high glucose levels.
What Happens If I Have Too Much Glucagon?
A rare tumor called a glucagonoma can cause the production of too much glucagon. When your body makes too much glucagon, glucose isn't stored for energy. Instead, it remains in your bloodstream, leading to high blood sugar levels and symptoms of diabetes.
What Happens If You Don't Have Enough Insulin or Glucagon?
In comparison, low insulin and glucagon levels can also cause health problems.

Too little insulin is a problem usually seen in people with diabetes. They can have problems producing insulin or using insulin effectively. In type 2 diabetes, the body can still make insulin, but it may not make enough, and/or insulin resistance has developed.
With type 1 diabetes, a person may make very little or no insulin whatsoever. Without enough insulin, your body can’t move glucose from the bloodstream into the cells. This results in high blood sugar levels and a lack of energy in the cells.
Symptoms of low insulin in type 1 diabetes can include weight loss, fatigue, dehydration, and confusion. Therefore, people with type 1 diabetes need to inject insulin to prevent these symptoms, which can be life-threatening.
It is very rare not to produce enough glucagon, but it is sometimes seen in babies or can result from removing the pancreas, weight loss surgery, or diabetes.
How to Monitor Your Insulin and Glucagon Levels
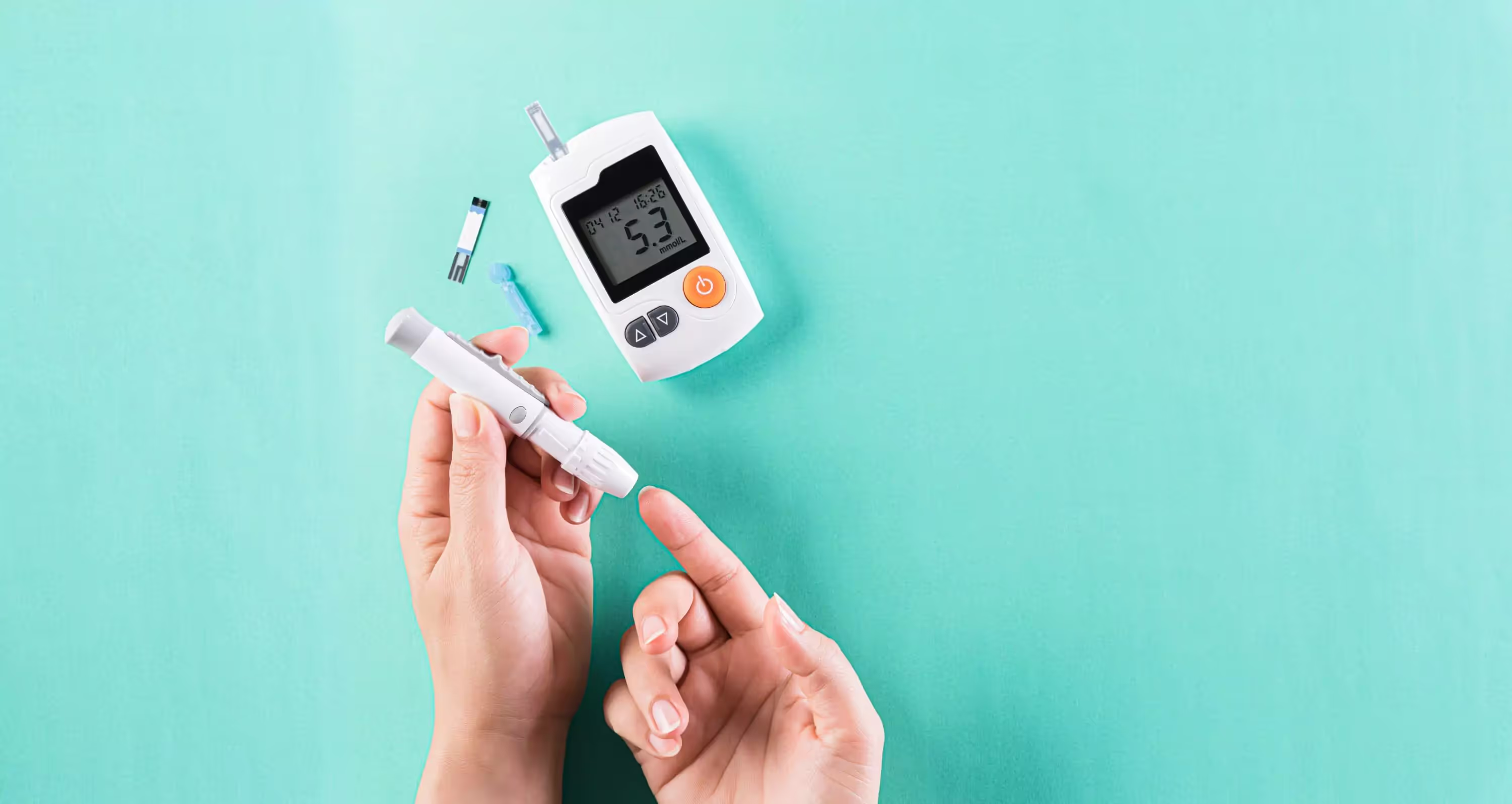
Although you can’t directly monitor your insulin and glucagon levels at home, you can monitor your glucose levels with a continuous glucose monitor (CGM), providing you with the data you need to understand if there is a problem with these hormones.
Find the right Nutrisense programto turn insight into progress.
Frequently Asked Questions
Is insulin anabolic or catabolic?
Insulin is an anabolic hormone. This means it promotes growth by helping your cells take up glucose to use as energy or store for future use. It also plays a role in producing proteins and fatty acids.
Does glucagon break down glycogen?
Yes. Glucagon signals your liver and muscle cells to break down stored glycogen back into glucose through a process called glycogenolysis. This glucose is then released into your bloodstream to raise glucose levels when they get too low.
Where are insulin and glucagon produced?
Insulin and glucagon are produced in the pancreas. Specifically, beta cells in the pancreas release insulin, while alpha cells release glucagon to maintain a steady supply of energy in your body.
Go Beyond Glucose Data with Nutrisense
Your glucose can significantly impact how your body feels and functions. That’s why stable levels are an important factor in supporting overall wellbeing. But viewing glucose isn't enough. Nutrisense, you’ll be able to learn how to use your body's data to make informed lifestyle choices that support healthy living.
One-to-one coaching
Sign up to access insurance-covered video calls to work with a glucose expert: a personal registered dietitian or certified nutritionist who will help tailor your lifestyle and diet to your goals.
Monitor and measure what matters
With the Nutrisense CGM Program, you can monitor your glucose with health tech like glucose biosensors and continuous glucose monitor (CGM)s, and analyze the trends over time with the Nutrisense App. This will help you make the most informed choices about the foods you consume and their impact on your health.
Find your best fit
Ready to take the first step? Start with our quiz to find the right Nutrisense program to help you take control.

Kara Collier is a registered dietitian nutritionist and certified nutrition support clinician who is passionate about reshaping how we approach prevention, behavior change, and metabolic health. A Forbes 30 Under 30 honoree, she’s helped over 150,000 people improve their metabolic health using tools like continuous glucose monitors and behavior-focused nutrition strategies. Kara has been featured by Forbes, UC Berkeley, and HLTH, and has appeared on top podcasts like Mind Pump and The Genius Life.