Postprandial Blood Sugar: Normal Levels and How to Optimize Them

Key Takeaways
- Postprandial glucose levels: Postprandial glucose refers to your blood sugar concentration after eating, with a normal 2-hour measurement typically falling below 140 mg/dL for healthy adults.
- Post-meal glucose response: Factors such as carbohydrate intake, protein balance, sleep quality, and physical activity all influence how effectively your body manages glucose after a meal.
- Glucose monitoring: Tracking your individual response with a glucose biosensor and a Registered Dietitian can reveal specific triggers and help you maintain stable metabolic health.
- Postprandial glucose levels: Postprandial glucose refers to your blood sugar concentration after eating, with a normal 2-hour measurement typically falling below 140 mg/dL for healthy adults.
- Post-meal glucose response: Factors such as carbohydrate intake, protein balance, sleep quality, and physical activity all influence how effectively your body manages glucose after a meal.
- Glucose monitoring: Tracking your individual response with a glucose biosensor and a Registered Dietitian can reveal specific triggers and help you maintain stable metabolic health.
There are a variety of factors that can affect how your blood sugar changes after a meal besides just the foods you eat. Things like sleep quality, exercise, and even stress levels all play a unique role.
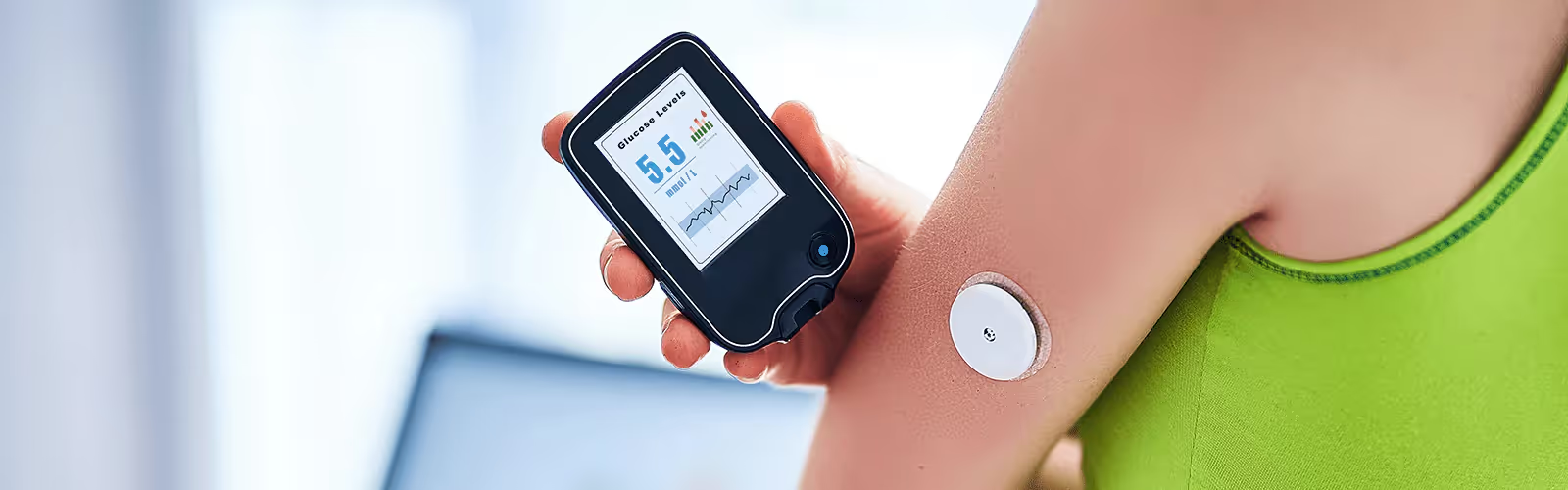
Optimal blood sugar levels are an important facet of metabolic health, so it’s important to understand how and why they can fluctuate. Monitoring your postprandial blood sugar levels, or your post-meal glucose response in two hours after eating is one way to do so.
These levels allow you to measure how well your body is able to release insulin into the bloodstream to use and store glucose. But how can postprandial blood sugar be measured? And do certain foods affect it differently?
In this article, we’ll dig into how your blood sugar changes after you eat, why postprandial blood sugar is important to measure, and share some tips to improve your blood sugar after your meals.
The Fed-Fast Cycle and Metabolism
The fed-fast cycle of metabolism is made up of four main stages: fed, post-absorptive, fasting, and prolonged fasting. Each stage refers to a part of the eating cycle and the processes occurring within the body while it digests food and converts it into energy.
Let’s break each one of these states down to better understand what their function is and how they relate to blood sugar.
1) Fed (Absorptive State)
The fed state of this cycle is the period of time about two to four hours after a meal. This is when your body digests and absorbs all the nutrients from your food.
During this time, glucose enters the bloodstream, proteins are broken down, and insulin is released by the pancreas to help your body use glucose for energy and store excess amounts.
Postprandial blood sugar is measured during this stage to determine how your glucose levels have risen. This measurement can indicate how effective your body is at using and storing glucose, and it can also detect low insulin sensitivity and even indicate an increased risk of diabetes.
Aside from insulin and glucose related functions, your body undergoes other functions during this state:
- Releasing bile from gallbladder to help with fat digestion
- Digesting soluble, fermentable fiber from your meal
- Releasing proteins to help carry nutrients to tissues and organs
2) Post-Absorptive (Early Fasting State)
Once your body has absorbed all the nutrients and carried out the main digestive functions, it enters the postabsorptive state. This typically begins around four hours after eating and can extend another 12-18 hours if no more food is consumed.
During this state, glucose levels can dip to as low as 70 mg/dL (or 4.4 mmol/L) in healthy adults as insulin returns to its basal level. To produce more energy, the liver starts a process called glycogenolysis. During this process, glycogen stored in the liver is broken down to be converted into glucose and used for energy.
The early fasting state extends overnight for most people, since no food is consumed for eight or more hours during sleep. If this state is prolonged, however, your liver may start to produce ketones and enter the fasting state.
3) Fasting State

The fasting state begins when your body has completely absorbed, digested, and stored the nutrients from your last meal. This period begins after about 18 hours and can span up to two full days without eating.
Fasting is sometimes grouped together with the postabsorptive state, but the amount of time gone without eating is the important distinction. In the fasting state, glycogen has usually been fully depleted and the body begins to rely on gluconeogenesis for fuel.
Ketogenic amino acids released by muscle protein breakdown will be converted into ketones and allow the brain, heart, and skeletal muscles to adapt to using these if the fasting continues. When the fasting period ends, the body will utilize fat and protein to replenish stores that were drained, and glucose is sent to the peripheral tissues before returning to the liver.
4) Prolonged Fasting State
The final state, which is known as starvation, is rarely reached by the average person as it requires more than 48 hours without eating. The body will conserve proteins that are vital for life, but more extensive internal protein breakdown will occur in this stage to be converted into glucose.
At this stage, the body will use up the majority of its fuel stores and shift from gluconeogenesis to lipolysis and rely on ketone bodies for fuel. Fatty acids become the primary fuel for the heart, liver, and skeletal muscle, while the brain will adapt to using ketones for fuel.
What is a Normal 2-Hour Postprandial Blood Sugar?

For most healthy adults, a blood glucose measurement under 140 mg/dL (7.8 mmol/L) is a normal for postprandial blood sugar. In individuals who have diabetes, prediabetes, or insulin resistance, your postprandial blood sugar levels may be elevated to around 180 mg/dL.
Preprandial blood glucose, or your blood sugar level before eating, should fall somewhere between 70 to 130 mg/dL according to the American Diabetes Association.
Why is Monitoring Your Postprandial Blood Sugar Important?
Monitoring your postprandial blood sugar allows you to understand how well your body responds to insulin, how your glucose levels fluctuate, and to get a better overall view of your metabolic health.
While it isn’t the only marker to be aware of when it comes to glucose metabolism, it’s an important one. Research has shown that postprandial blood sugar levels are strongly associated with HbA1c levels, meaning they are better indicators of glycemic control.
Postprandial hyperglycemia can indicate a higher risk for developing type 2 diabetes or cardiovascular disease. This refers to blood sugar levels that consistently rise above 140 mg/dL in the hours after eating. Detecting abnormal postprandial levels can also help you implement new dietary or lifestyle changes that can help lower your risk of developing these conditions.
Ways to Check Your Postprandial Blood Sugar
Now that you understand why monitoring postprandial blood sugar can be important, here are three of the best ways to check your levels.
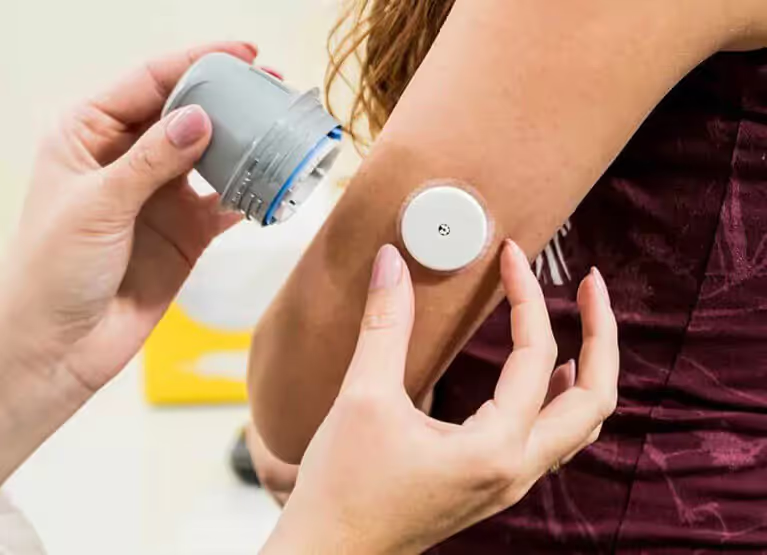
Continuous Glucose Monitoring (CGM)
A CGM can provide great insight into your metabolic health by tracking your blood sugar levels throughout the day. You can monitor three trends: fasting glucose, postprandial (post meal glucose), and glycemic variability (the "swings" in your glucose).
A higher fasting glucose value (anything above 99 mg/dL) can be indicative of insulin resistance. An abnormally high number can also indicate the development of prediabetes or diabetes.
A higher postprandial value can be used to determine whether your body is bringing glucose down to baseline efficiently. Recent studies suggest that this value is actually more effective in determining the risk of cardiovascular conditions than fasting glucose.
Oral Glucose Tolerance Test (OGTT)
The oral glucose tolerance test (OGTT) is also known as the glucose tolerance insulin response (GTIR) test. The OGTT helps practitioners determine how quickly glucose is cleared from the blood, and has been used to screen for glucose dysfunction.
This test tests your fasting glucose level and then tests your level every hour after you drink a glucose beverage to observe how your blood sugar responds. The Nutrisense Nutrition Team uses and recommends the GTIR. Your dietitian can best guide you through this test and the optimal lab values for you.
Self-Monitoring Blood Glucose (SMBG)
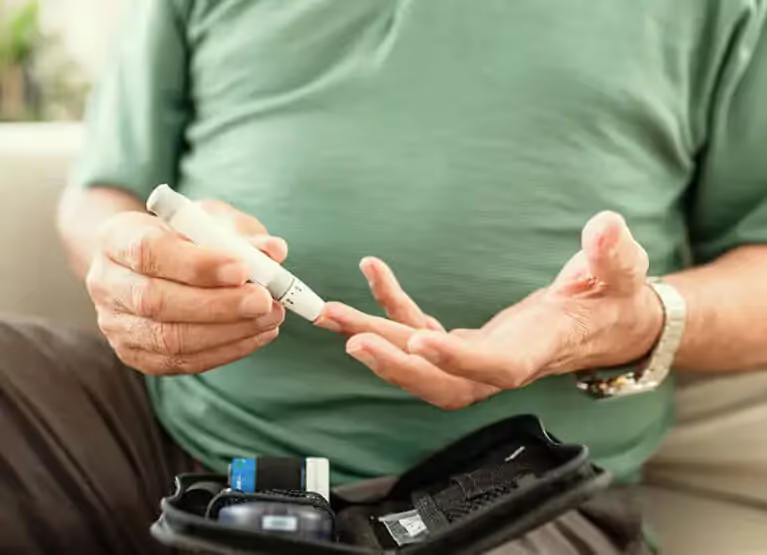
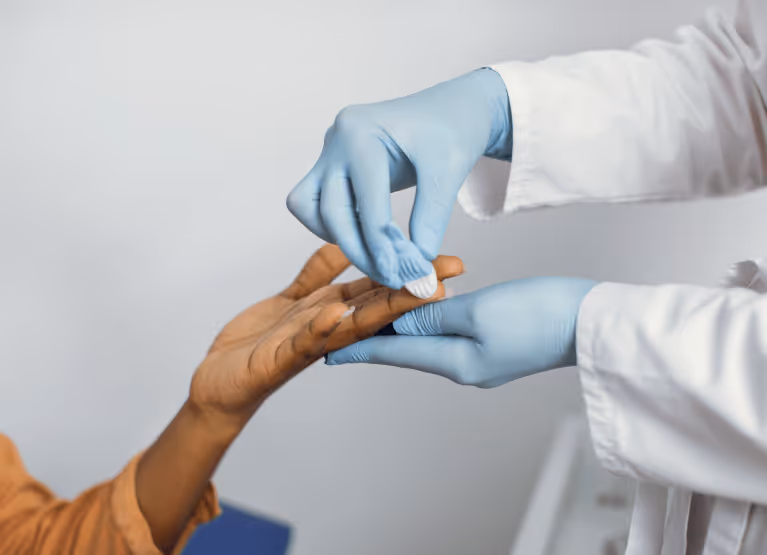
Self-monitoring your blood glucose levels can be measured using a glucometer. This test, also known as the finger-prick method, involves pricking your finger using a lancet. A drop of blood from the prick is then placed onto a strip so that the glucometer can measure the amount of glucose attached to your blood cells.
One key difference between the finger prick method and CGM is that the finger prick method measures whole blood whereas a CGM gathers data from interstitial fluid.
Factors that Influence Postprandial Blood Sugar Levels
Once you start monitoring your postprandial blood sugar levels, you may notice abnormal responses, blood sugar spikes, or fluctuations that can be a result of many factors.
Carbohydrate Intake

High postprandial blood sugar levels can damage your metabolic health over time. So, one way to reduce this negative impact is to determine how many carbohydrates you need to consume.
There’s no one-size-fits-all recommendation for carb intake, and the exact amount will differ for everyone. For some, a low-carb keto diet may work best to regulate blood sugar levels. For others, lifestyle factors such as exercise can also play an important role and require you to consume more carbs.
The best way to figure this out is to take an individualized approach. Working with a dietitian or nutritionist, using a continuous glucose monitor to monitor your levels, or using a diet tracking app are all ways to determine how many carbs are optimal for you.
The type of carbohydrates you consume are also important. While refined carbohydrates like sugar and white bread are known for their effect on glucose, even some complex carbohydrates may result in suboptimal glucose responses. However, eating your carbs with a source of fiber or protein is a great way to help blunt any potential glucose spikes.
How Much Protein You Eat
Protein helps prevent glucose spikes by slowing down digestion. Including lean protein sources like chicken breast, tofu, edamame, fish, Greek yogurt, beans, and legumes can help support optimal glucose levels.
It’s important to note, however, most studies have shown no benefit for improved glucose regulation when consuming higher amounts of protein above estimated needs. The key is to focus on finding the right balance of protein, carbohydrates, and fats for your unique body. This where an individualized approach either with a CGM, dietitian, or both can help.
Quality of Sleep

Getting adequate sleep is good for overall health but can also help increase insulin sensitivity by reducing stress and mitigating inflammation. Plus, don’t you feel amazing when you’ve had a night of really good sleep?
Not getting enough sleep is a risk factor for developing insulin resistance. In fact, a study found that even a week’s worth of sleep deprivation results in reduced insulin sensitivity. You may find your postprandial blood sugar levels improve as your sleep quality improves.
Amount of Daily Exercise
Exercising regularly will help your body respond to insulin, which again may help your body better regulate blood glucose levels after meals. A large body of research has shown that exercise increases insulin sensitivity.
In individuals with type 2 diabetes, getting exercise after eating has even been shown to improve postprandial glucose levels. Going out for a run, hike, jog, or meeting friends to play a sport together are all great ways to get more steps in and support better glucose levels.
Find the right Nutrisense programto turn insight into progress.
Frequently Asked Questions
What are normal postprandial glucose levels?
Normal postprandial glucose levels for most healthy adults are generally below 140 mg/dL (7.8 mmol/L) when measured two hours after a meal. This range indicates that the body is effectively releasing insulin to clear glucose from the bloodstream. Consistently higher readings may suggest insulin resistance or a higher risk of metabolic health conditions.
How can you lower postprandial glucose levels?
You can lower postprandial glucose levels by prioritizing fiber and protein, engaging in light physical activity after eating, and ensuring adequate sleep. Walking for 10-15 minutes post-meal helps muscles utilize glucose more efficiently. Additionally, managing stress and understanding individual carbohydrate tolerance can significantly reduce the magnitude of post-meal glucose spikes.
What is the best postprandial blood glucose measurement time?
The standard postprandial blood glucose measurement time is two hours after the start of a meal. This window allows your body enough time to begin digesting nutrients and for insulin to respond. Monitoring 24/7 with a glucose biosensor provides even greater detail, revealing the peak timing and duration of your individual glucose response.
Go Beyond Glucose Data with Nutrisense
Your glucose can significantly impact how your body feels and functions. That’s why stable levels are an important factor in supporting overall wellbeing. But viewing glucose isn't enough. Nutrisense, you’ll be able to learn how to use your body's data to make informed lifestyle choices that support healthy living.
One-to-one coaching
Sign up to access insurance-covered video calls to work with a glucose expert: a personal registered dietitian or certified nutritionist who will help tailor your lifestyle and diet to your goals.
Monitor and measure what matters
With the Nutrisense CGM Program, you can monitor your glucose with health tech like glucose biosensors and continuous glucose monitor (CGM)s, and analyze the trends over time with the Nutrisense App. This will help you make the most informed choices about the foods you consume and their impact on your health.
Find your best fit
Ready to take the first step? Start with our quiz to find the right Nutrisense program to help you take control.

Heather is a Registered and Licensed Dietitian Nutritionist (RDN, LDN), subject matter expert, and technical writer, with a master's degree in nutrition science from Bastyr University. She has a specialty in neuroendocrinology and has been working in the field of nutrition—including nutrition research, education, medical writing, and clinical integrative and functional nutrition—for over 15 years.