Why Consumer CGM Use is Good for Diabetics

Key Takeaways
It can be a perfectly natural knee-jerk response to think that any new group of people using a technology takes something away from the early adopters. In the case of continuous glucose monitors (CGMs), the ultimate early adopters would be people with diabetes mellitus of any variety.
Diabetes mellitus, otherwise known as either type 1 (T1DM) or type 2 diabetes (T2DM), is hallmarked by elevated blood glucose or blood sugar, and monitoring glucose levels is essential for these populations. In T1DM, the body stops producing enough insulin, which normally instructs cells to take glucose up from the blood.
In type 2 diabetes, meanwhile, the body stops responding to the insulin it does produce. In either case, much of the long-term damage done by the disease is caused by all that glucose trapped in the blood.
CGMs first allowed people with these conditions to monitor their glucose levels constantly, informing them when best to use external insulin, for example. If blood glucose levels spiked after a meal, they would know about it as soon as possible if they had a CGM. This is just one of the many benefits of using a CGM.
As these devices proved so essential for management of diabetes mellitus, uptake was relatively fast and widespread. Like most new medical technologies, what had started as a specialized tool quickly became a ubiquitous part of healthcare management.
Today, it is pretty rare to see a person with diabetes mellitus who hasn’t been made aware of the option to use a CGM by their healthcare provider. With each generation of CGMs, some people are inevitably made aware of the devices for the first time, bringing them into the total market.
{{rich-text-cta-3="/style-guide"}}
More People Can Access CGMs
Ultimately, this is good for everyone who needs them since the more CGMs that are produced, the cheaper they are to make per individual CGM. As a result, there are now several types of CGM devices and over-the-counter glucose biosensors that can match a person’s unique needs and preferences better than a single product.
In the field of economics, this effect is known as an economy of scale. We won’t bore you with the details, but the take-home message is that producing a thousand CGMs at once costs much less than making a single CGM a thousand times. As mentioned above, the broad uptake of CGMs has also led to different options for people who need or want them.
But what does all this mean for someone who has been using a CGM from the first generation, for example? Have the benefits of using a CGM stayed the same?
For the early adopter, in this case, someone who started using a CGM many years ago when they were first developed for people with diabetes mellitus, the total cost of using a CGM has been reduced by wider use. This is a robust economic trend that we feel is all but likely to continue as CGMs become used by the general population, much like any other technology.
It’s also worth bearing in mind that some newer CGMs also have much longer replacement cycles than their predecessors. The result is that, in addition to lower total costs for CGMs, someone with diabetes mellitus now has a wide range of choice in terms of software, hardware, price, style, and frequency of replacement. The last one can be pretty important for people who don’t like the idea of using and disposing of technological products for ecological and financial reasons.
Improving the Visibility and Acceptance of CGMs
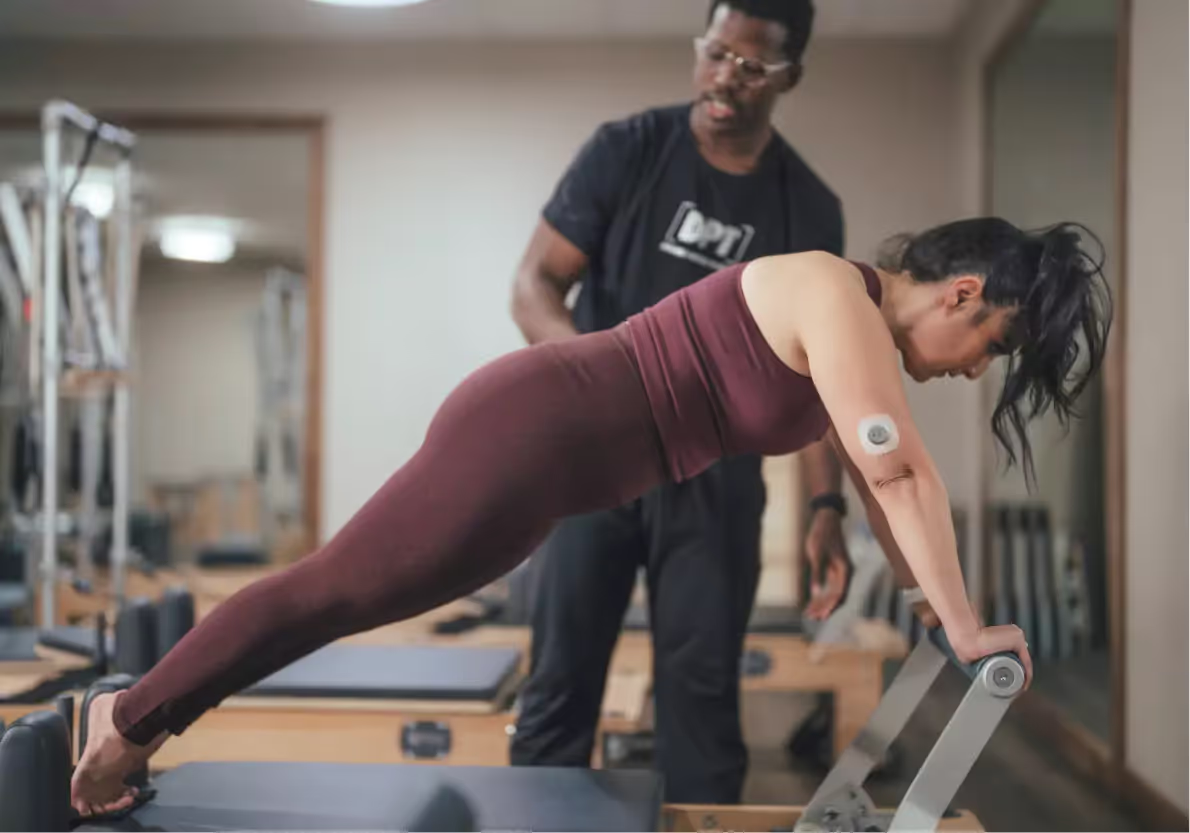
Put as simply as possible, there is generally a stigma associated with diseases—this is an unfortunate reality that we all hope will ameliorate over time. There is also a doubly harmful stigma associated with illnesses that other people may perceive are a product of personal choices one makes over a lifetime.
Although T1DM is simply an unfortunate lack of insulin production, one that is no individual person’s responsibility, T2DM is sadly often seen as an inevitable consequence of a person’s food and exercise decisions.
The truth is that someone’s life and management of any conditions they may have throughout their life is the combined result of genetics, food and exercise decisions, and treatments available to them. Seeing someone with a CGM as of a decade or so ago may have been a marker, for ignorant people, of poor decisions that person may have supposedly made in the past.
When used by the public, some of the first adopters of CGMs have historically been athletes and people in generally excellent health, fully aware of a wide range of personal health data and how to use it effectively. Although it isn’t the first thing we think of here, we consider it a nice side effect that CGMs are coming to be seen as a marker of good health and proactive health management, rather than something only necessary for specific conditions.
In a similar sense, people may first see CGMs used by athletes and good health advocates, which we would also consider a good result for a first impression. This also drives the cycle above, in which new users who never would have known about CGMs drive the cost down for everyone.
Find the right Nutrisense programto turn insight into progress.
Go Beyond Glucose Data with Nutrisense
Your glucose can significantly impact how your body feels and functions. That’s why stable levels are an important factor in supporting overall wellbeing. But viewing glucose isn't enough. Nutrisense, you’ll be able to learn how to use your body's data to make informed lifestyle choices that support healthy living.
One-to-one coaching
Sign up to access insurance-covered video calls to work with a glucose expert: a personal registered dietitian or certified nutritionist who will help tailor your lifestyle and diet to your goals.
Monitor and measure what matters
With the Nutrisense CGM Program, you can monitor your glucose with health tech like glucose biosensors and continuous glucose monitor (CGM)s, and analyze the trends over time with the Nutrisense App. This will help you make the most informed choices about the foods you consume and their impact on your health.
Find your best fit
Ready to take the first step? Start with our quiz to find the right Nutrisense program to help you take control.

Kara Collier is a registered dietitian nutritionist and certified nutrition support clinician who is passionate about reshaping how we approach prevention, behavior change, and metabolic health. A Forbes 30 Under 30 honoree, she’s helped over 150,000 people improve their metabolic health using tools like continuous glucose monitors and behavior-focused nutrition strategies. Kara has been featured by Forbes, UC Berkeley, and HLTH, and has appeared on top podcasts like Mind Pump and The Genius Life.



.avif)
