How to Improve Insulin Sensitivity Naturally: 9 Evidence-Based Ways

Key Takeaways
- Natural ways to improve insulin sensitivity: Evidence-based lifestyle changes like optimizing your carbohydrate intake, engaging in regular exercise, and reducing systemic inflammation are highly effective.
- Dietary impact on insulin resistance: Identifying the right complex carbohydrates for your body and balancing them with adequate protein and healthy fats helps cells respond better to glucose.
- Lifestyle factors beyond food: Managing chronic stress, prioritizing sleep, and getting enough daily sunshine for vitamin D are critical for long-term metabolic health.
- Natural ways to improve insulin sensitivity: Evidence-based lifestyle changes like optimizing your carbohydrate intake, engaging in regular exercise, and reducing systemic inflammation are highly effective.
- Dietary impact on insulin resistance: Identifying the right complex carbohydrates for your body and balancing them with adequate protein and healthy fats helps cells respond better to glucose.
- Lifestyle factors beyond food: Managing chronic stress, prioritizing sleep, and getting enough daily sunshine for vitamin D are critical for long-term metabolic health.
Insulin resistance, or or the condition where your body no longer responds to insulin as well, is a little tricky, is a little tricky. Your glucose lab results may look “fine,” but you may still find yourself experiencing energy fluctuations, post-meal carb comas, and excess adipose tissue (or fat) that won’t budge, especially around your midsection.
Why is insulin sensitivity so important? Many health conditions and issues aside from high blood sugar and belly fat can be associated with insulin resistance, including:
- Obesity
- Heart Disease
- Polycystic Ovary Syndrome (PCOS)
- High Blood Pressure
Some common causes include:
- Family history or genetics
- Visceral fat, or general excess weight or body fat
- Poor diet
- Inactivity
- Secretion of the stress hormone
While detecting the exact cause of insulin resistance can be challenging, there’s a way you can get to the bottom of whether this is the root of your health problems.
Read on to see how to detect insulin resistance and learn more about nine ways to improve insulin sensitivity for better metabolic health.
How to Determine Insulin Resistance
Testing for insulin resistance isn’t as straightforward as testing for prediabetes or diabetes, for which your doctor would request a fasting glucose or HbA1c (hemoglobin A1c test).
Insulin resistance is a complex physiological change that occurs over years and is hallmarked by two changes:
- Being an increase in insulin levels (hyperinsulinemia)
- Decreased insulin sensitivity in our cells.
One option is to take the glucose tolerance insulin response, or GTIR, test (also called the oral glucose tolerance test). It's a functional test you can discuss with your functional medicine practitioner or registered dietitian nutritionist. The Nutrisense Nutrition Team uses and recommends this test. Your dietitian can best guide you through the oral glucose tolerance test and the optimal lab values for you.
Another option is the HOMA-IR, another functional test with varying optimal levels depending on factors such as age and gender (although used in research, this test isn’t often seen in clinical practice).
Unfortunately, there isn't one single test to assess if we are insulin resistant or not. The best test is called a Hyperinsulinemic-Euglycemic Clamp and is very invasive. Because of that, it is only used in research settings. So instead, we have to look at the bigger picture with multiple factors involved. The Nutrisense Nutrition Team recommends to assess the following:
- CGM data: this can provide great insight into your metabolic health. Here you and your dietitian will want to monitor three trends: fasting glucose, postprandial (after meal) glucose, and glycemic variability (the "swings" in glucose). A higher fasting glucose value can be indicative of impaired fasting glucose and insulin resistance (in both the liver and muscle), so we want to see values between 70-90. A higher after meal value can tell us if insulin isn't bringing glucose down to baseline quickly or effectively enough.
- Fasting insulin levels: Similar to fasting glucose levels, this tells us some information about our insulin but only provides a snapshot into what's happening in a fasted state. We want to see fasting insulin levels between 2-8.
- HDL: aim for values > 60.
- Triglycerides: aim for values <90.
- TG to HDL ratio should be <1.
- Waist circumference: <40 inches for men and <35 inches for women.
- Blood pressure: aim for values < 120/80.
- ALT & AST: aim for values 20 or less.
- hsCRP: this gives us a good indication of general inflammation. Make sure not to exercise right before the test. Aim for values < 1.
- Uric acid: aim for values <5.
Nine Ways to Improve Insulin Sensitivity
As the American Diabetes Association notes, you can focus on improving insulin resistance. To do this, you’re essentially focusing on how to make your body’s cells more receptive to insulin.
This includes getting more physical activity, dietary improvements, and weight loss if you have excess body fat or obesity issues.
Take a look at some effective ways to improve insulin sensitivity, so you maintain a healthy weight, feel energized, and notice an improvement in your overall wellness.
1) Optimize Your Carbohydrate Consumption

Because insulin resistance involves having high levels of this hormone “floating around” in your blood, it’s likely that it’s not getting to your cells properly.
Insulin signals to the body to let glucose in. But if your body isn’t listening to insulin, it will be much harder for glucose to get in leading to high blood glucose levels in your blood. And high glucose levels, over time, can damage your metabolic health.
So, one way to reduce this negative impact is to optimize your carbohydrate consumption. Eat the amount of carbohydrates that will be right for you and be the right amount for your body to take in.
Of course, there’s no perfect carb intake, and the exact amount will differ for everyone. For some, a general low-carb diet may work best, while for others, it will depend on various other lifestyle and dietary factors.
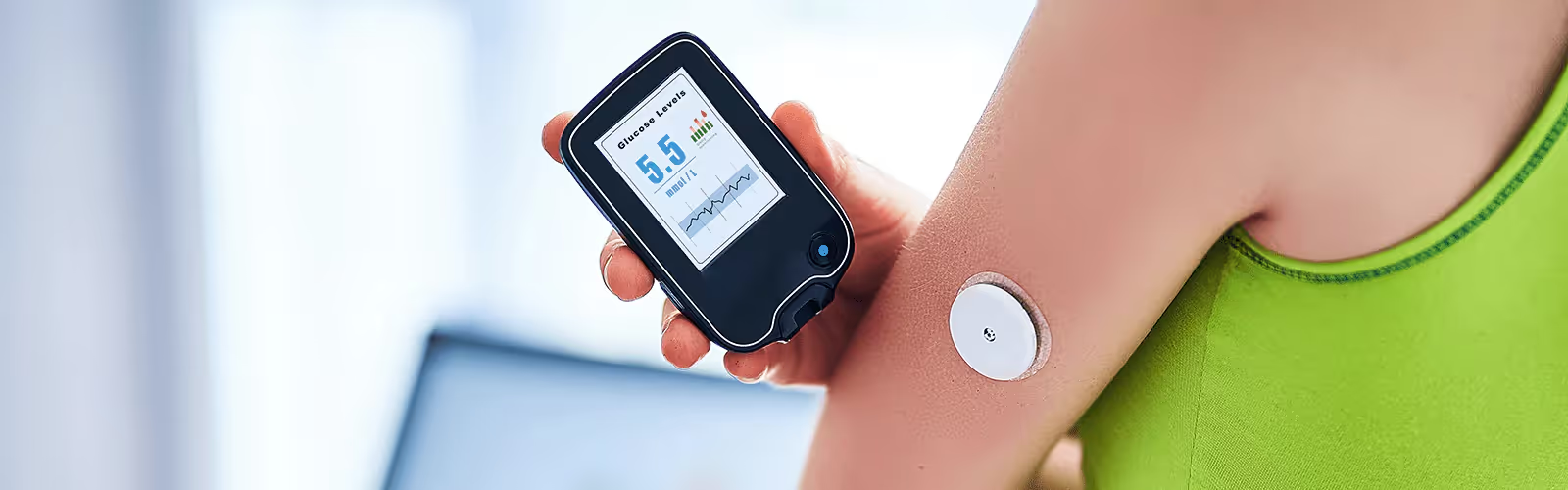
The best way to figure this out is to take an individualized approach. It can mean working with your nutritionist, using a device like a continuous glucose monitor to monitor your glucose levels, or DIY-ing the process yourself with a meal journal and health tracker.
Optimizing carbohydrate consumption can be a great approach to take at the beginning while you work with your healthcare team to get to the root of the issue, which is encouraging your body to respond to the insulin.
2) Identify the Best Carbohydrates for You
Naturally, after optimizing your carbohydrate intake, you’ll want to figure out which carbohydrates are right for you.
Even some healthy carbohydrates may result in suboptimal glucose responses (if you’re tracking with a CGM device). So it’s less about what’s considered healthy and more about what works best for you.
That said, some foods will unsurprisingly result in suboptimal responses. One example is refined carbohydrates, which often result in blood sugar spikes and crashes, especially if you don't pair them with enough healthy fats and/or protein.
This can also help with better glucose levels as you try other tips to help your body respond to insulin.
3) Engage in Exercise

This tip will help your body respond to insulin. Do you get enough physical activity? It helps prevent more than just weight gain! A large body of research has shown that exercise increases insulin sensitivity.
Moreover, exercise can also increase muscle mass, and increased muscle mass takes more glucose out of the blood and into the cells.
And the weight loss you experience from exercise will also help boost insulin sensitivity. It's because there’ll be less fat and less inflammation (from high levels of fat) competing with insulin to get into the cells in your body.
4) Get the Right Amount of Protein and Fat for You
Protein helps prevent glucose spikes by slowing down digestion. But too much protein can backfire and reduce insulin sensitivity.
Similarly, a diet high in fat and refined carbohydrates can contribute to insulin resistance too. However, pairing your carbohydrates with a little bit of fat can help with improving blood glucose levels.
The key is to focus on finding the right balance of protein, carbohydrates, and fats for your unique body. This where an individualized approach either with a CGM, dietitian, or both can help.
5) Consider the Effect of Inflammation

Chronic inflammation creates an environment where many harmful molecules prevent your body from responding to insulin. One reason for inflammation is high body fat levels since adipose tissue holds onto inflammatory molecules.
And as we mentioned, losing weight through exercise is a great way to reduce inflammation and improve insulin sensitivity.
Another way is to live an anti-inflammatory lifestyle, including focusing on antioxidant-rich fruits and vegetables, cutting down on trans fatty acids, avoiding spending too much time in polluted areas, reducing exposure to obesogens, and engaging in healthier habits. We discuss some of these habits below!
6) Get Some Sunshine
Spending time in the sun for a safe length of time is one healthy lifestyle habit that can improve vitamin D levels and insulin sensitivity.
One study found that getting an adequate amount of bright sunshine was linked to reduced insulin resistance. The researchers illustrated this link by showing that healthy sun exposure resulted in decreased fasting insulin levels.
And sunlight exposure was also found to improve LDL, cholesterol, and triglyceride levels, helping to decrease the risk of type 2 diabetes in this study.
7) Boost Micronutrients in Your Diet

Yet another healthy lifestyle habit that is tied to eating antioxidant-rich fruits and vegetables! Antioxidants are a type of micronutrient that help to eliminate harmful inflammatory and stressful molecules from the body.
Other micronutrients that can help improve insulin sensitivity include:
- Magnesium, found in chocolate and avocado.
- Plenty of fiber, found in fruits and vegetables.
- Whole protein sources that are rich in amino acids such as L-carnitine, taurine, and L-arginine such as pasture raised eggs and poultry.
- Cruciferous vegetables such as broccoli, cauliflower, and Brussel sprouts, are rich in insulin sensitivity-improving glutathione.
8) Reduce Stress Levels
Too much stress can encourage insulin resistance. Reducing stress helps to reduce inflammation, helps regulate hunger, and can help to keep your glucose levels stable too.
According to Diabetes UK, stress results in high levels of hormones such as cortisol and adrenaline. These hormones, like inflammatory molecules, will make it harder for your body to respond to insulin properly.
Here are some tips to reduce stress:
- Engage in mindfulness.
- Try meditation.
- Block off time in your schedule for “me time.”
- Take daily walks.
- Set boundaries.
- And incorporate the other tips already mentioned, such as getting sunlight and eating an inflammatory, micronutrient-rich diet.
9) Get Enough Sleep

Getting adequate sleep is good for overall health but can also help increase insulin sensitivity by reducing stress and mitigating inflammation. Plus, don’t you feel amazing when you’ve had a night of really good sleep?
Not getting enough sleep is a risk factor for developing insulin resistance. In fact, a study found that even a week’s worth of sleep deprivation results in reduced insulin sensitivity.
So, it may be time you used your boundary-setting skills with yourself to get to bed on time and catch those Zs. Here’s a sleep hygiene checklist to get you started in the right direction.
Find the right Nutrisense programto turn insight into progress.
Frequently Asked Questions
How do you increase insulin naturally?
You generally want to improve how your body uses insulin, rather than increasing production naturally. The pancreas automatically releases insulin in response to food, but improving your cellular sensitivity through diet, exercise, and sleep ensures your body needs less of it to manage glucose effectively.
What does increased insulin sensitivity mean?
Increased insulin sensitivity means your cells are highly responsive to the hormone insulin. This is a positive metabolic state where your body efficiently moves glucose out of your bloodstream and into your cells for energy, reducing the risk of fat storage and chronic disease.
Is high insulin sensitivity good?
Yes, high insulin sensitivity is an indicator of excellent metabolic health. When your cells are sensitive, it prevents the pancreas from overworking and keeps circulating insulin levels low, which is crucial for maintaining stable energy and managing weight.
Go Beyond Glucose Data with Nutrisense
Your glucose can significantly impact how your body feels and functions. That’s why stable levels are an important factor in supporting overall wellbeing. But viewing glucose isn't enough. Nutrisense, you’ll be able to learn how to use your body's data to make informed lifestyle choices that support healthy living.
One-to-one coaching
Sign up to access insurance-covered video calls to work with a glucose expert: a personal registered dietitian or certified nutritionist who will help tailor your lifestyle and diet to your goals.
Monitor and measure what matters
With the Nutrisense CGM Program, you can monitor your glucose with health tech like glucose biosensors and continuous glucose monitor (CGM)s, and analyze the trends over time with the Nutrisense App. This will help you make the most informed choices about the foods you consume and their impact on your health.
Find your best fit
Ready to take the first step? Start with our quiz to find the right Nutrisense program to help you take control.

Jordyn has a bachelor’s degree in biology, a graduate degree in Human Nutrition and completed a dietetic internship at the Memphis VA. She's a dietitian at Nutrisense, and has experience working as a clinical dietitian at a VA medical center specializing in oncology and at the Mayo Clinic, working with a wide range of patients ranging from neonates in the NICU to adult ICU.