Can Hyperglycemia Cause a Stroke? Risks and How High Glucose Impacts the Brain

Key Takeaways
- Hyperglycemia and stroke: Chronic high glucose levels can damage blood vessels over time, leading to fatty deposits or clots that significantly increase the risk of an ischemic stroke.
- Stroke severity: High glucose levels during or after a stroke are associated with worse clinical outcomes, as they can increase brain tissue damage, acidosis, and inflammation.
- Stroke-like symptoms: Severe hyperglycemia can occasionally mimic stroke symptoms, making glucose monitoring and personal data interpretation essential for distinguishing metabolic issues from cardiovascular events.
- Hyperglycemia and stroke: Chronic high glucose levels can damage blood vessels over time, leading to fatty deposits or clots that significantly increase the risk of an ischemic stroke.
- Stroke severity: High glucose levels during or after a stroke are associated with worse clinical outcomes, as they can increase brain tissue damage, acidosis, and inflammation.
- Stroke-like symptoms: Severe hyperglycemia can occasionally mimic stroke symptoms, making glucose monitoring and personal data interpretation essential for distinguishing metabolic issues from cardiovascular events.
According to the World Health Organization, more than 15 million people per year suffer from stroke. Stroke is also the leading cause of death after heart disease, and the single most common cause of long-term disability.
So, it’s safe to say that the prevalence of stroke is a serious health issue. But what exactly causes someone to have a stroke? Does stroke severity have any connection to hyperglycemia?
Read on to learn everything you need to know about the effect of hyperglycemia on stroke and what factors can lead to this condition.
What are the Warning Signs or Symptoms of Hyperglycemia?
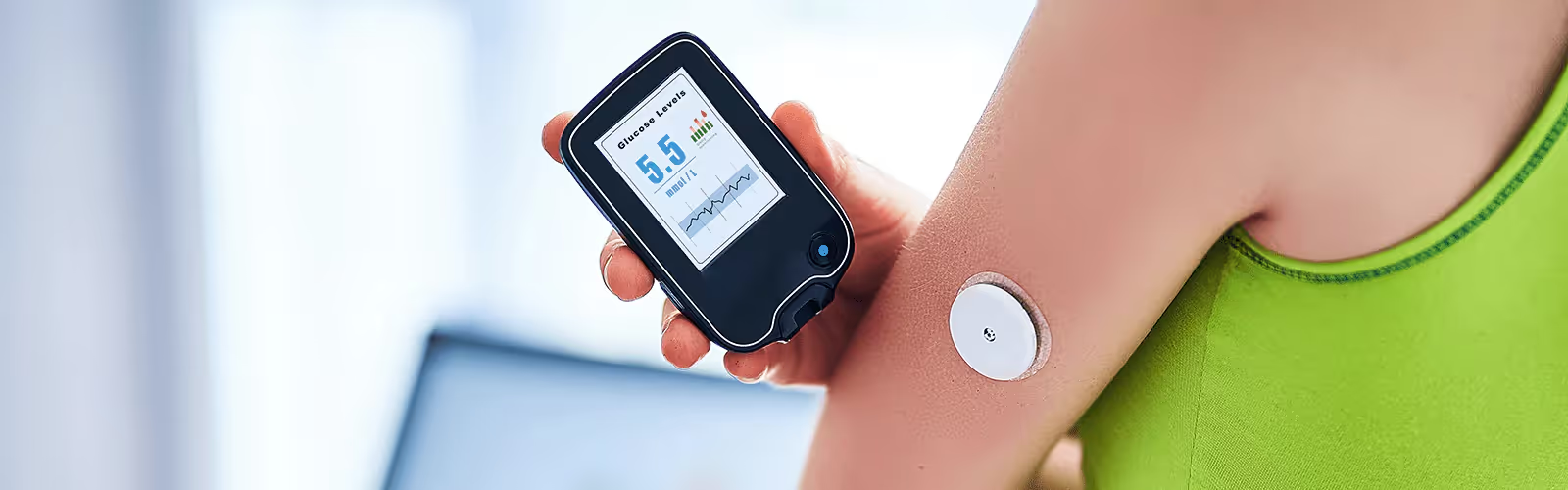
Hyperglycemia, or high blood sugar, can happen to anyone, even if you don’t have diabetes. That’s why it’s important to be familiar with the symptoms.

Some of the early symptoms of hyperglycemia can include things like:
- High blood sugar
- Increased thirst and/or hunger
- Blurred vision
- Frequent urination
- Headache
- Feeling weak or tired
- Weight loss
- Slow-healing cuts and sores
Once you’re familiar with the common symptoms, you may be wondering if there is anything that may put you more at risk of developing hyperglycemia. The risk factors for hyperglycemia include:
- Having a family history of type 2 diabetes
- Being African American, Native American, Hispanic or Asian American
- Being overweight
- Having high blood pressure or cholesterol
- Having polycystic ovarian syndrome (PCOS)
- Having a history of gestational diabetes, a form of diabetes that occurs when pregnant and usually goes away after the birth of the baby
Hyperglycemia vs. Diabetes
Hyperglycemia and diabetes are closely related, but they aren’t exactly the same thing. Hyperglycemia occurs when there is too much sugar in the blood.
Here’s how it works:
- When you eat, some of your food is converted into glucose in your body, which is sent into your bloodstream to be used.
- But, if glucose enters the bloodstream quicker than it can be used, your blood sugar level can spike to unhealthy levels.
- Chronic hyperglycemia can lead to health problems like insulin resistance, which can lead to type 2 diabetes.
Diabetes mellitus, on the other hand, is a group of metabolic diseases that involve chronic hyperglycemia. It is either caused by the body’s inability to produce or respond to insulin, or in some cases, both.
Insulin, a hormone released by the pancreas, plays a key role in allowing the glucose from your blood to move into your cells and be used up as energy.
If your body can’t make or use insulin, the glucose stays in your blood. This can lead to poor outcomes for certain health conditions over time.
People with type 1 diabetes produce little or no insulin, which is thought to be caused by an autoimmune response in the body. This condition destroys the cells in the pancreas that produce insulin.
Type 1 diabetes is not currently preventable, and is most often diagnosed in children, teens, and young adults. About five to 10 percent of people with diabetes have this type of diabetes.
People with type 2 diabetes can’t respond properly to the insulin their body makes. This leads to poor glycemic control and can result in a condition called insulin resistance. Type 2 diabetes is most often diagnosed in adults, but it is now also commonly being diagnosed in children, teens, and young adults.
About 90 to 95 percent of people with diabetes have type 2. It can often be prevented with certain lifestyle changes such as appropriate exercise, healthy eating, stress management, and weight management.
Can Hyperglycemia Cause Stroke?
You’re now familiar with the causes and risk factors of hyperglycemia. So, how might this condition be connected to strokes?
Having chronic high blood sugar can eventually result in increased fatty deposits or clots in blood vessels. These clots can narrow or block blood vessels in the neck or brain, which cuts off the blood supply.
This stops oxygen from getting to the brain, which can result in a hyperglycemic stroke.
How Does Hyperglycemia Increase the Risk of Stroke?
High blood sugar, or hyperglycemia can increase the risk and be an independent predictor of stroke over time. This condition is also associated with worse outcomes after a stroke.
Hyperglycemia is also observed to worsen some of the symptoms of stroke including:

- Acidosis, or too much acid in body fluids
- Accumulation of reactive oxygen species, which can cause brain damage after stroke
- Inflammation
- Mitochondrial dysfunction, which causes mitochondria to work less efficiently than they should. Mitochondria are a part of our cells which carry oxygen and convert food to energy in the body.
- Increasing final infarct size, which is the area of tissue death caused by blood vessel blockage during stroke
For these reasons, acute stroke patients with hyperglycemia or hypertension tend to have more complications than those without these conditions.
What Happens in the Brain During Stroke?
As we mentioned earlier, stroke happens when the blood supply to part of the brain is blocked, or when a blood vessel in the brain bursts. During stroke, parts of the brain become damaged or die.
Stroke can cause lasting brain damage, long-term disability, or even death. To work properly, our brains need oxygen, which is delivered by the blood that is pumped into all parts of the brain through our arteries.
If something blocks this flow, your brain cells can start to die within minutes, causing stroke.
Types of Stroke
There are two different types of stroke: ischemic strokes and hemorrhagic strokes. There is also something called a transient ischemic attack or TIA, which is sometimes called a ministroke.
Ischemic Stroke

Ischemic stroke is the most common type of stroke. It happens when the blood vessels in your brain are narrowed or blocked, causing severely reduced blood flow and oxygen flow, or ischemia.
In ischemic stroke patients, blocked or narrowed blood vessels are caused by fatty deposits that build up in blood vessels. Sometimes, blood clots or other debris traveling through the bloodstream, most often from the heart, can lodge in the blood vessels in the brain and cause stroke.
Hemorrhagic Stroke
Hemorrhagic stroke is caused by a burst or leaking blood vessel in the brain. It is often related to a condition that affects the blood vessels, like:
- Uncontrolled high blood pressure
- Overtreatment with blood thinners
- Aneurysms, or bulges at weak spots in your blood vessel walls
- Trauma to the body, such as a car accident
- Cerebral amyloid angiopathy, which are protein deposits in blood vessel walls that lead to weakness in the vessel wall
- An acute ischemic stroke that leads to hemorrhage
Transient Ischemic Attack (TIA)
A transient ischemic attack, or TIA, is a temporary period of symptoms similar to those in a stroke. It’s sometimes referred to as a ministroke.
It is caused by a temporary decrease in blood supply to part of the brain, which may last as little as five minutes. It usually occurs when a clot or debris reduces or blocks blood flow to the brain.
A TIA doesn’t necessarily cause permanent damage, but it can increase your risk of having a full-blown stroke. It isn’t possible to tell if you’re having a TIA or stroke just from symptoms.
It’s best to always seek advice from a healthcare professional immediately, even if your symptoms have gotten better.
Other Medical Conditions that Can Increase the Risk of Stroke

Hyperglycemia isn’t the only condition that can increase your risk for stroke onset. Here are seven more health conditions that may be linked to stroke.
Previously Had a Stroke or TIA
Having a TIA or stroke can increase your chances of having another stroke. In fact, one in four stroke survivors may go on to have another stroke.
Research indicates that most people who have experienced ischemic stroke will need medication that prevents another.
The American Heart Association recommends maintaining the following to reduce the risk of a second stroke:
- Maintaining healthy blood sugar levels
- Monitoring your cholesterol levels
- Following a well-balanced diet
- Getting plenty of exercise
High Blood Pressure
High blood pressure can increase your risk of stroke by damaging arteries throughout the body. This creates conditions in which they can burst or clog more easily.
Hypertension is the number one cause of stroke and studies suggest that maintaining a healthy blood pressure can reduce your stroke risk.
High Cholesterol

Cholesterol is a fatty substance that your body needs to function properly. However, high levels of cholesterol in the body can cause fatty deposits to build up in your arteries.
This can cause your arteries to stiffen, and make it harder for blood to flow through, increasing the risk of stroke. It can also increase the risk of blood clot formation, which can also increase the risk of stroke.
Though genetics play a role in your cholesterol levels, other diet and lifestyle factors may impact it as well.
Heart Disease
Heart disease can increase your risk for stroke. Coronary heart disease, for example, can cause plaque to build up in your arteries, blocking the flow of oxygen-rich blood to the brain.
Other heart disorders like heart valve defects, irregular heartbeat, and enlarged heart chambers can increase the risk of blood clots, which are also linked to increased risk of stroke.
Diabetes
Research shows that people with diabetes may be up to three times more likely to have a stroke compared to others. Diabetes can also cause hyperglycemia and high blood pressure, both of which are also linked to an increased risk of stroke.
Obesity

Obesity, or excess body fat, is linked to high cholesterol, diabetes, and high blood pressure, all of which can increase the risk of stroke. Maintaining a healthy BMI may be one way to lower your risk of suffering from a stroke.
Sickle Cell Disease
Sickle cell disease causes some red blood cells in the body to form an abnormal sickle shape. This can increase the likelihood that cells will get stuck in blood vessels, blocking the flow of blood to the brain and causing a stroke.
Find the right Nutrisense programto turn insight into progress.
Frequently Asked Questions
What blood sugar level causes stroke?
There is no single glucose level that causes an immediate stroke, but chronic hyperglycemia above 126 mg/dL significantly increases long-term risk. Persistently high glucose damages arterial walls, leading to the formation of clots that can block blood flow to the brain. Monitoring your individual response with 24/7 data can help identify patterns that increase cardiovascular risk.
Can hyperglycemia cause stroke-like symptoms?
Yes, severe hyperglycemia can occasionally mimic stroke symptoms, a condition sometimes referred to as a "pseudostroke." Extremely high glucose levels can cause neurological disturbances such as confusion or weakness that resemble the warning signs of a true stroke. Consult a healthcare professional immediately if you experience these symptoms to ensure an accurate diagnosis.
What is the connection between glucose and stroke level?
High glucose levels are an independent predictor of stroke and can worsen the recovery process after a cardiovascular event occurs. Acute hyperglycemia can increase acidosis and oxidative stress in the brain, leading to larger areas of tissue death. Working with a Registered Dietitian to stabilize glucose variability is a key strategy for long-term stroke prevention.
Go Beyond Glucose Data with Nutrisense
Your glucose can significantly impact how your body feels and functions. That’s why stable levels are an important factor in supporting overall wellbeing. But viewing glucose isn't enough. Nutrisense, you’ll be able to learn how to use your body's data to make informed lifestyle choices that support healthy living.
One-to-one coaching
Sign up to access insurance-covered video calls to work with a glucose expert: a personal registered dietitian or certified nutritionist who will help tailor your lifestyle and diet to your goals.
Monitor and measure what matters
With the Nutrisense CGM Program, you can monitor your glucose with health tech like glucose biosensors and continuous glucose monitor (CGM)s, and analyze the trends over time with the Nutrisense App. This will help you make the most informed choices about the foods you consume and their impact on your health.
Find your best fit
Ready to take the first step? Start with our quiz to find the right Nutrisense program to help you take control.

Heather is a Registered and Licensed Dietitian Nutritionist (RDN, LDN), subject matter expert, and technical writer, with a master's degree in nutrition science from Bastyr University. She has a specialty in neuroendocrinology and has been working in the field of nutrition—including nutrition research, education, medical writing, and clinical integrative and functional nutrition—for over 15 years.