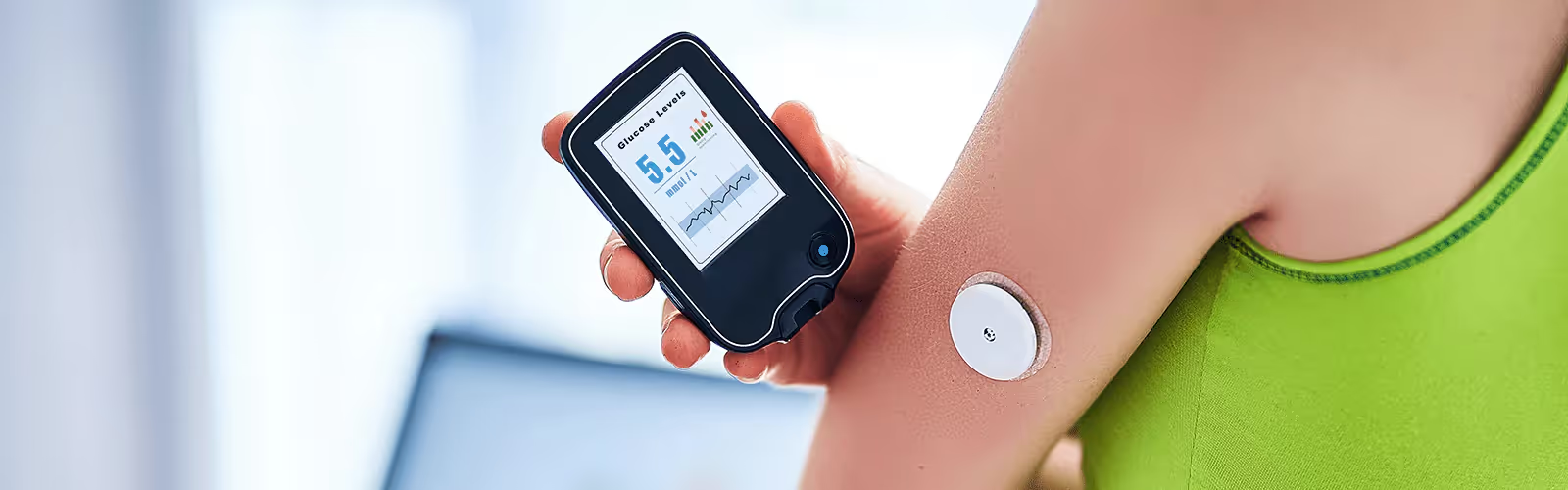
Blood Sugar and Inflammation: How Glucose Spikes Drive Cellular Stress

Key Takeaways
- Blood sugar and inflammation: High glucose levels can trigger an immune response by increasing oxidative stress and the production of pro-inflammatory cytokines.
- Glucose spikes and inflammation: Rapid fluctuations in your glucose levels, often called spikes, can damage cellular health and contribute to chronic systemic inflammation.
- Diabetes and inflammatory markers: Chronic inflammation is both a cause and a consequence of insulin resistance, creating a cycle that can increase the risk of type 2 diabetes.
- Blood sugar and inflammation: High glucose levels can trigger an immune response by increasing oxidative stress and the production of pro-inflammatory cytokines.
- Glucose spikes and inflammation: Rapid fluctuations in your glucose levels, often called spikes, can damage cellular health and contribute to chronic systemic inflammation.
- Diabetes and inflammatory markers: Chronic inflammation is both a cause and a consequence of insulin resistance, creating a cycle that can increase the risk of type 2 diabetes.
The relationship between blood glucose and inflammation is complex but interesting. We’re sure you already have a ton of questions about it: Does inflammation raise insulin? Is there a link to diabetes, like an increased risk of developing it? And if you don’t already know enough about inflammation, there are many reasons why you should.
For starters, people with diabetes or pre-diabetes could benefit from learning more about it since inflammatory molecules can directly affect how your body processes sugars and fats. And there’s helpful information here for non-diabetic people too! After all, knowing more about things like immune responses, the markers of inflammation, and the links between insulin resistance and inflammation can help optimize your health.
Research shows that inflammation plays a vital role in regulating blood glucose levels. When scientists first made this discovery, it led to things like anti-inflammatory drugs that target the immune system and treat type 2 diabetes. Today, we know more about how these medications work, and we’re able to better control blood glucose levels with them than we were in the past.
Learning more about inflammation and blood glucose will also help you learn how to minimize your risk of cardiovascular disease, high blood pressure, heart disease, and cholesterol. Here are some insights so you can begin to understand more about how best to track, monitor, and make changes to optimize your health.
What You Need to Know About Inflammation

Inflammation is a natural process—it’s commonly thought of as your body’s response to viruses, infections, and injury. It’s your body attempting to defeat a threat, and it’s usually a good thing. Without inflammation, even simple ailments could cause damage, but this protects your body from harm under normal conditions.
How Does Inflammation Occur?
Before we dive into the links between inflammation and blood glucose, it’s a good idea to learn more about how inflammation occurs. At its core, your body is a complex system of various parts that work together like a well-oiled machine. When something happens—like an infection or an injury—specialized cells address these issues.
In other words, when something bad happens within your body, there are systems in place designed to fix those problems for you. This is great from an evolutionary standpoint, since it was crucial for human survival thousands of years ago when there wasn’t much support or focus on preventive health.
So, when your body faces an injury, infection or any other type of stressor, your immune system jumps into action, sending messengers to fight off danger. These stressors can include anything from an environmental toxin to a dietary trigger.
However, these messengers stay active for too long or get sent out too frequently in some people. This can cause chronic low-level inflammation. This then contributes to insulin resistance, making it difficult for your body to process sugar (glucose). If you suffer from high blood sugar due to insulin resistance, you may be more at risk of several health issues. These can include heart disease, high cholesterol, blood pressure issues, nerve damage, blindness, and kidney problems.
The Types of Inflammation
There are two types of inflammation: acute and chronic. Here’s a little more about what you need to know about each type:
Acute Inflammation
This is a short-term response and occurs in response to an injury or infection. It happens immediately after you’re physically injured or when you get a cold or the flu. It can be painful but usually passes within a few days once your body resolves whatever problem sets off its response. This type comes with pain, swelling, warmth, redness, tenderness, or even constant itching or tingling.
Chronic Inflammation
According to orthopedic spine surgeon Dr. Carl Giordano, "chronic inflammation is a low-grade inflammation that can persist for months or even years. It is associated with a variety of chronic diseases, including heart disease, stroke, cancer, and Alzheimer's disease. While inflammation is a natural part of the body's healing process, chronic inflammation can damage tissues and organs over time."
Chronic inflammation may occur because of untreated infections. Or it could occur because of acute inflammation from an injury that you didn’t address in time. Some cases of chronic inflammation can also be the result of prolonged exposure to pollution or toxins in the air.
However, there’s some chronic inflammation that may not have a definitive cause. You usually see it as a low-level of inflammation that spreads slowly through your body. This type of systemic inflammation can lead to auto-immune diseases like arthritis.
Both acute and chronic inflammation are essential when it comes to healing injuries. But too much of either type can be harmful. Acute inflammation can be a good thing if it means getting over a respiratory or gastrointestinal infection. Chronic inflammation, however, is more often associated with poor health outcomes. There are various reasons for it, and the links between inflammation and other risk factors (like high levels of visceral fat and aging) are key to understanding exactly how the process works.
Inflammation and Blood Glucose Levels

The links between inflammation and blood glucose are complex, and research is still ongoing. However, there’s a clear link between high glucose and diabetes with elevated inflammatory markers. So, let’s try and break it all down.
When we talk about diabetes and pre-diabetes, it’s easy to only think about high blood sugar levels. But inflammation also affects our cells. It makes them insulin resistant, leading to chronically elevated blood sugar levels. Inflammation is often called a “silent” condition. This means it can develop unnoticed over time, contributing to chronic diseases like type 2 diabetes.
In a nutshell, when you eat foods high in sugar or high-glycemic carbohydrates, you trigger an inflammatory response. This is why some experts raise concerns about diets that are high in processed foods. They can lead to inflammation-related issues like obesity, heart disease, cancer, diabetes, Alzheimer’s disease...and even depression.
So, whether you’re aiming for weight loss or trying to prevent a decline in glucose tolerance, information about inflammation is essential. And, to monitor and deter hyperglycemia or the development of other side effects, being aware of the links between inflammation and blood glucose levels is a good idea. This is where non-diabetic glucose monitoring using a CGM can come in handy.
A Cycle of Inflammation and Blood Glucose Responses
Inflammation is also often associated with stress. Increased cortisol from stress (internal or external) can decrease insulin sensitivity and increase hepatic glucose output. This molecule is endocrinologically active and produces a short-term response to raised blood glucose levels. Remember, you can manage sources of stress easier if your body has more energy to use, so this spike isn’t always a bad thing. However, chronic stress can lead to higher glucose levels, which can increase inflammatory processes in the body.
Elevated blood glucose levels can lead to the production of free radicals, or molecules that lack an electron, ‘stealing’ one from nearby molecules to stabilize their own structures. But we’re not going to get into biochemistry about how all of that works.
What you need to know is these are pro-inflammatory. This inflammatory state can adversely affect already elevated blood glucose levels. Lipid peroxidation—a more scientific term for the process of free radicals oxidizing fat molecules—is another side effect of high blood glucose levels, leading to chronic inflammatory conditions. Over time, the ability of the pancreas to respond to these spikes in blood glucose levels decreases, so smaller amounts of glucose will produce stronger spikes, quickening the cycle.
Inflammation, Aging, and Blood Glucose

There’s already a link between aging and blood glucose levels, so what happens when inflammation enters the mix? Researchers are still studying the connection between things like hyperglycemia, diabetes, aging, and inflammation, like in this study by the American Diabetes Association (ADA).
Still, inflammation and aging are so closely linked that some researchers prefer to use the term “inflamm-aging” to describe the endless loop they seem stuck in. It refers to chronic, low-level, or background inflammation. This can occur because of insufficient sleep, overeating, a sedentary lifestyle, and chronic stress compounded over many years of your life. Remember that as you age, you may also become less active, leading to weight gain. This adds our next point to the mix—fat tissue.
Inflammation and High Levels of Fat Tissue
Inflammation affects and is affected by so many things, it’s no surprise weight gain and weight loss also makes a difference. Take being overweight, for instance. It can make it harder for you to control your blood glucose. This is because high levels of fat tissue can cause low-grade inflammation, which may negatively impact glucose levels.
Research indicates that among older people and those with diabetes, there were higher levels of two pro-inflammatory cytokines compared to those in younger, non-diabetic people. Cytokines are small proteins that help with cell signaling. These cytokines (measured after an overnight fast) were linked to aging, diabetes, and increased truncal fat mass. This suggests they were at least in part produced by that central, visceral fat.
There are many steps you can take to reduce inflammation and improve overall health. Losing weight or making sustainable lifestyle changes isn’t always easy. But it can be worth it: losing even 5% of your body weight may reduce your risk of developing diabetes.
What You Can Do to Prevent and Manage Inflammation

It’s a good idea to get regular checkups and track and monitor your health to see whether inflammation may already be affecting you. If it is, a medical professional will help you find a solution to help you reduce or control it.
According to Dr. Giordano, here are some tips to consider to help you reduce inflammation from dietary and lifestyle sources:
- Include anti-inflammatory foods such as cherries, berries, and other colorful fruits, vegetables, and foods rich in antioxidants in your diet.
- Get plenty of sleep (at least seven to nine hours per night).
- Manage your stress levels with coping strategies like meditation and breathing techniques.
- Try to cut down on or avoid eating too many refined carbohydrates, sugars, trans fats, and processed foods.
- Limit or avoid tobacco and alcohol use.
- Maintain a healthy weight.
- Get plenty of physical activity. Try engaging in things like moderate aerobic and weight-bearing exercises three to five times a week.
Find the right Nutrisense programto turn insight into progress.
Frequently Asked Questions
Does high blood sugar cause inflammation?
Yes. Elevated glucose levels can increase oxidative stress and the production of pro-inflammatory cytokines. Tracking your individual glucose response can help identify dietary patterns that may trigger this immune reaction.
Does diabetes cause inflammation?
It can. Diabetes is frequently characterized by chronic, low-grade systemic inflammation. This inflammatory state often worsens insulin resistance, creating a cycle that can further elevate glucose levels over time.
Is diabetes an inflammatory disease?
Many researchers consider type 2 diabetes to have a strong inflammatory component. Chronic inflammation plays a significant role in the development and progression of insulin resistance, which is a hallmark of the condition.
Go Beyond Glucose Data with Nutrisense
Your glucose can significantly impact how your body feels and functions. That’s why stable levels are an important factor in supporting overall wellbeing. But viewing glucose isn't enough. Nutrisense, you’ll be able to learn how to use your body's data to make informed lifestyle choices that support healthy living.
One-to-one coaching
Sign up to access insurance-covered video calls to work with a glucose expert: a personal registered dietitian or certified nutritionist who will help tailor your lifestyle and diet to your goals.
Monitor and measure what matters
With the Nutrisense CGM Program, you can monitor your glucose with health tech like glucose biosensors and continuous glucose monitor (CGM)s, and analyze the trends over time with the Nutrisense App. This will help you make the most informed choices about the foods you consume and their impact on your health.
Find your best fit
Ready to take the first step? Start with our quiz to find the right Nutrisense program to help you take control.

Kara Collier is a registered dietitian nutritionist and certified nutrition support clinician who is passionate about reshaping how we approach prevention, behavior change, and metabolic health. A Forbes 30 Under 30 honoree, she’s helped over 150,000 people improve their metabolic health using tools like continuous glucose monitors and behavior-focused nutrition strategies. Kara has been featured by Forbes, UC Berkeley, and HLTH, and has appeared on top podcasts like Mind Pump and The Genius Life.