Glucose & Stress: How Monitoring Can Help Improve Stress Levels

Key Takeaways
- Stress-related glucose changes: During the fight-or-flight response, hormones like cortisol and adrenaline signal the liver to release stored glucose, causing rapid spikes.
- Glucose as a metabolic stressor: Extreme glucose fluctuations and states of insulin resistance act as internal physiological stressors that increase your overall metabolic burden.
- Biosensor data for sleep and energy: Tracking your 24/7 glucose patterns helps identify how daily stressors impact your energy levels, allowing you to optimize your routine.
- Stress-related glucose changes: During the fight-or-flight response, hormones like cortisol and adrenaline signal the liver to release stored glucose, causing rapid spikes.
- Glucose as a metabolic stressor: Extreme glucose fluctuations and states of insulin resistance act as internal physiological stressors that increase your overall metabolic burden.
- Biosensor data for sleep and energy: Tracking your 24/7 glucose patterns helps identify how daily stressors impact your energy levels, allowing you to optimize your routine.
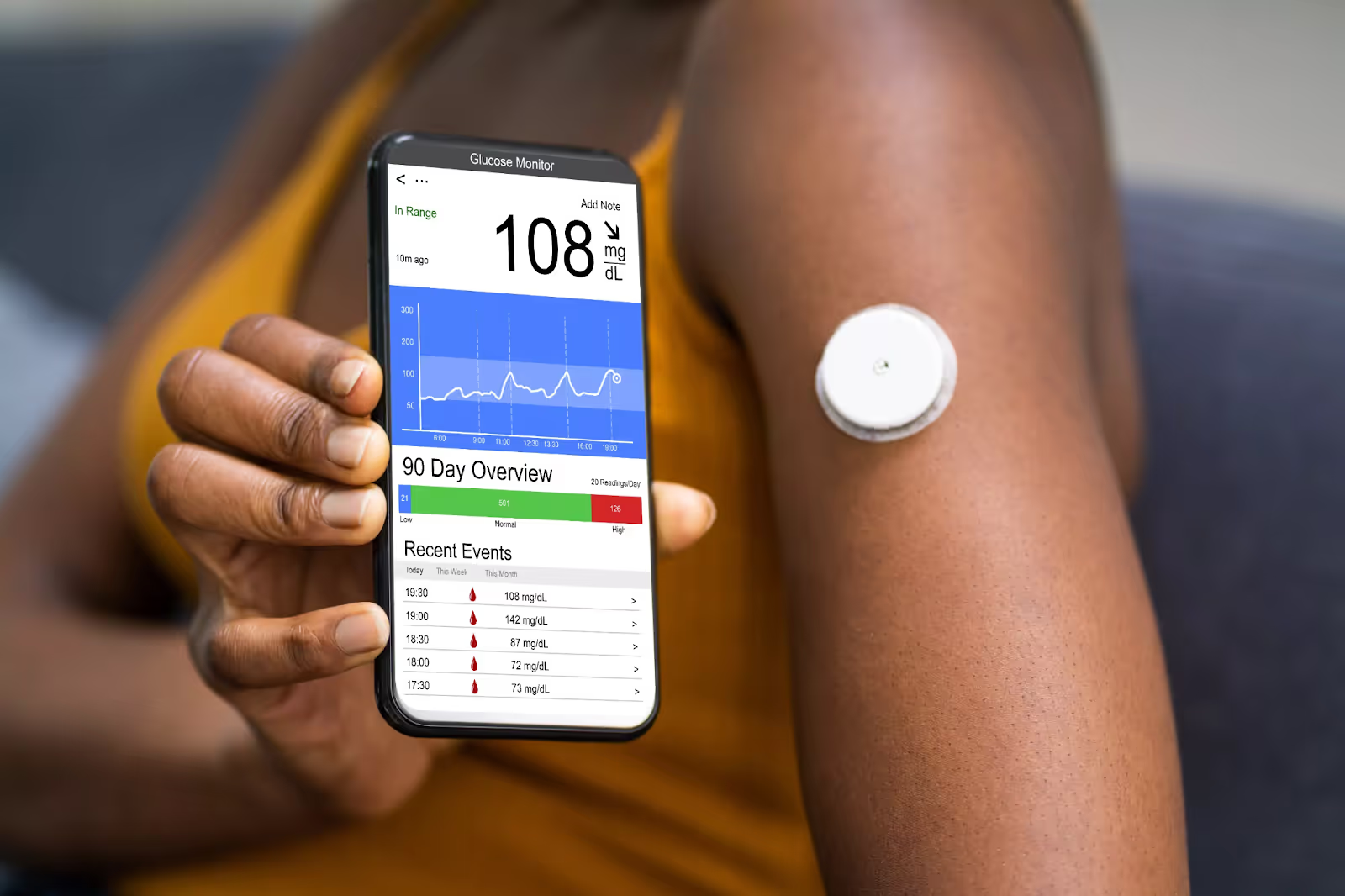
Stress directly impacts your glucose, and unstable glucose adds to your body's stress load. Monitoring your glucose with a biosensor that measures glucose in interstitial fluid reveals this connection, showing how your body responds and giving you the data to manage your stress and energy levels.
Key Points:
- During the body's 'fight or flight' response, hormones like adrenaline and cortisol can cause a spike by signaling the liver to release stored glucose.
- Explore the 'How to Manage & Reduce Stress' section below for practical techniques like breathing exercises and improving sleep hygiene.
- The Nutrisense program uses over-the-counter biosensors, meaning a prescription is not required to get started.
How are Stress and Glucose Connected?
You've probably heard people say that stress can make you sick. But does all stress make us sick? And what is really meant by the word "stress,” anyway?
Stress impacts everybody in different ways, and surprisingly, your glucose levels can be impacted during times of high stress. So what happens to our glucose response when we experience stress, and how do our glucose levels in turn impact our body's ability to process and manage stress?
Stress and glucose have an intimate two-way relationship, and it's important to understand this relationship so we can hack it at the deepest level. To kick us off, let's take a closer look at what stress really is and how it works in our bodies.
What is Stress in the Body?

First, we must admit: not all stress is bad! Some of it is actually good.
Stress is simply a type of pressure applied to a system. Whether something is a “good” or “bad” pressure or stressor depends on the dose and the timing.
Dose and Timing
When we are building and maintaining our bone density, load-bearing exercise or resistance training is a stress applied to our bones and connective tissue. In most people, this pressure will stimulate bone growth - a good thing.
Similarly, when we are young and our immune system is developing, we are exposed to all kinds of stress in the form of pathogens from the outside world. These pathogen stressors train our immune system to recognize and protect against future invaders - also a good thing.
However, we can break a bone with too much load-bearing, and we can die from an infectious illness we didn’t have the ability to fight off. You can see that the difference between a stressor that helps or hurts is how and when we apply it and whether or not we have the internal ability to adapt to it.
Shared Biochemistry
All stressors, from “external sources” such as a fight with a loved one or “internal ones” such as a food intolerance, are interpreted by the same stress-response biochemistry in the body.
This is why we can say: all stress, regardless of its origin, is ultimately metabolic stress.
What are Common Stressors?
Stress placed on the body can occur along a continuum and is most commonly found in the form of:
- Emotional drama or trauma
- Physical activity/exercise
- Nutrient imbalances (both deficiency and excess may be detrimental), including glucose
- Intolerances to foods, medications, or supplements
- Injuries or infectious illnesses
- Environmental toxins/xenobiotic exposure
- Exposure to allergens
- Sleep deprivation
You may have noticed that glucose was on that list. How can glucose itself be a stressor? We'll talk about that in a minute! But first, let's look at some other things on this list.
Emotional Stressors
When most of us talk about stress, we are often referring to that first bullet point: emotional drama/trauma. Maybe you got into a fight with your best friend or find yourself worrying a lot about a situation at work.
Your brain and body don't really know the difference between these things and the primitive memory of being chased by a bear. It's all a response wired into the same system: the stress-response system, or neuroendocrine system. The neuroendocrine system is all about helping you adapt to a changing world and the changing pressures within it.
Part of how we evolved to adapt to stress involves increasing our stress hormone, cortisol, which in turn tends to increase glucose levels. This makes sense! The body needs more quick fuel to launch a sprint to safety or defense.
But these emotional stressors aren't the only stressors we have going on. Everything else on this list exerts equally important pressure on our metabolic framework - speeding up some chemical reactions, slowing others down - and perhaps overloading others into a biochemical traffic jam!
Can Glucose Act as a Stressor?
Glucose can itself be a stressor as well. Here's how we can create more overall metabolic stress when our glucose is out of whack:
Big Spikes
When glucose rises very high into the "danger zone" after, let's say, we've eaten a giant piece of birthday cake at 8 pm, this is registered as a significant metabolic stress on the body. To respond, the body will initiate a cascade of hormonal and molecular changes that work to bring the body back to homeostasis and "normal" glucose levels.
Insulin Resistance
Over time, and over repeated exposures to the higher stress of these more extreme glucose spikes, the body may fundamentally change how it responds to the incoming flood of glucose. And eventually, we may arrive at a state of insulin resistance.
This process of acquiring a maladaptive response (insulin resistance) is a bit more complex than we'll dissect here. But, you can see how we have used the metabolic pressure or stressor of too much glucose to trigger damage in the body that now alters an important aspect of our baseline metabolic health and function.
Impaired glucose regulation can impact many other areas of metabolic function. With insulin resistance itself, we see impaired stress regulation of other areas of the metabolic planet as well. Insulin resistance increases our risk for many diseases, all affecting metabolic health as a whole.
Lows and Symptoms
It's also possible to have a stress-response reaction triggered when glucose falls too low (hypoglycemia). Hypoglycemia can be a metabolic stressor that leads to symptoms such as worsened fatigue, anxiety, brain fog, headaches, and more.
How Do You Know if Stress is Impacting Your Glucose Levels?
As you can see on our two-way street, stressors coming in from non-glucose origins can impact glucose, and changes in glucose itself can impact the function of our stress-response system on a larger level. Changes in glucose can happen as a result of any change in our metabolic stress load from any one of these origins.
That Stressful Day and the Surprise Glucose Spike
You just wrapped up a tense 30-minute call for work. Your heart is still pounding, and you feel that familiar wave of exhaustion. You head to the kitchen and grab a handful of crackers to take the edge off.
An hour later, you glance at your data and see a sharp glucose spike that seems out of proportion for that small snack. This is where you can see the direct link between stress and your metabolism. The tense call prompted your body to release extra glucose, and the snack you ate afterward compounded the effect.
Monitoring Features To Spot Stress-Related Glucose Changes
Alerts and pattern views can make it simpler to see when stress may be affecting your readings. On compatible sensors and apps, you can set customizable alerts for out-of-range values, including a low glucose alarm. The Nutrisense App centers on pattern analysis and experiments that pair your 24/7 data with food, sleep, stress notes, and activity.
- Customizable alerts for high and low ranges on compatible sensors and apps
- Low glucose alarm for a quick check-in and log
- Pattern analysis charts in the Nutrisense App to review timing and variability alongside your logs
- No finger pricks, since sensors read glucose measured in interstitial fluid - see What is a CGM?
If data overload is a concern, schedule Insurance-covered video calls with a registered dietitian to review your patterns and decide on one or two next steps that fit your day.
Though it might initially feel overwhelming to consider all of these different sources of stress and wonder how we are supposed to turn this into simple, practical, daily action, it's easier than you might imagine!
What Symptoms Signal Stress?
Your body's response to different stressors likely won't be the exact same as someone else's response. With stress and glucose, one person's medicine is another's poison. For one person, we may see a longer fasting window improve glucose regulation and stress management, while for someone else, they may need a much shorter window to achieve optimal glucose response.
We can often use key symptoms like the following to interpret and gauge stress levels in our bodies:
- Low energy levels
- Poor mood or mood swings
- Poor sleep quality
- Impaired cognitive function
- Impaired digestive function
Personalized Tolerance
These symptoms can also help us determine where our individual tolerance is for different stressors.
Having a way to see our daily patterns in glucose response is a powerful tool in this process.
How Can You Manage Stress and Glucose?

There are lots of ways to try to reduce your stress levels, and finding your personal optimal “sweet spot” regarding stress takes some time and experimentation. Here are some tips:
Track Symptoms
Do you struggle with any symptoms such as fatigue, anxiety/depression, poor sleep, difficulty concentrating, poor digestion, body pain, or difficulty managing weight? If so, consider tracking how these symptoms may change from day to day as you experiment with some of the following:
Whole Foods First
Nutrients such as amino acids, fatty acids, vitamins, and minerals are all required by the metabolic “superhighways” in appropriate amounts and ratios in order to perform all of the functions of metabolism. This includes stress regulation!
Regardless of what dietary approach you follow, research shows that laying a strong foundation of nutrient density through whole foods first is best. You might consider working with a registered dietitian to help you discover what dietary approach meets your unique nutritional needs, including how to assess your tolerance or sensitivities to different foods and supplements.
Appropriate Exercise
Some people may need more or less physical activity than others. Don’t be afraid to experiment with different kinds of movement (including some solid rest days) and different types, intensities, and durations of exercise throughout the week to see what helps you feel your best.
Stay Hydrated
This is simple, but incredibly important. Make sure you're drinking plenty of water throughout the day. If you're not sure how much water you should be drinking, check out our article on dietitian-recommended hydration strategies.
Sleep Hygiene
Getting plenty of rest is important for everything from cognitive function to weight regulation. Here's what you need to know about sleep, stress, and your glucose.
Breathwork and Yoga
Practicing yoga and meditation are two great ways to slow your mind and body down to reduce stress. Here’s some more info on how to hack your cortisol with diaphragmatic breathing.
Find the right Nutrisense programto turn insight into progress.
Methods & Sources
This article summarizes current evidence on stress–glucose interactions and Nutrisense’s data-collection approach; methods and recent peer‑reviewed sources are listed below.
Methods
- Weight Loss Outcomes Methodology
- Personalized Guidance Outcomes Methodology
- Subjective Well-Being & Habits Survey
- Coaching & Weight Outcomes (Internal Data)
Peer-reviewed References
The stress response and glucose metabolism — Nature Reviews Endocrinology (2024). DOI/PMID: https://doi.org/10.1038/s41574-024-00912-4
Continuous glucose monitoring outside of diabetes: clinical utility and limitations — Nutrients (2024). DOI/PMID: https://doi.org/10.3390/nu16030789
Sleep, circadian rhythms, and glycemic regulation: 2024 consensus statement — The Lancet Diabetes & Endocrinology (2024). DOI/PMID: https://doi.org/10.1016/S2213-8587(24)00123-4
Author Credit
By Heather Davis, MS, RDN, LDN | Reviewed by Kara Collier, RDN, LDN, CNSC
Frequently Asked Questions
How can I use glucose biosensor data to improve sleep and energy?
You can use biosensor data to identify which stressors disrupt your glucose homeostasis. By monitoring your 24/7 glucose patterns alongside sleep and activity logs, you can pinpoint the specific lifestyle factors draining your energy. A Registered Dietitian can then help you build personalized habits to stabilize those responses.
Does stress cause glucose spikes?
Yes. When you experience emotional or physical stress, your neuroendocrine system releases cortisol and adrenaline to prepare for action. These hormones signal your liver to release stored glucose into your bloodstream, which can cause significant glucose spikes even if you haven't eaten.
Can low glucose trigger a stress response?
Yes, hypoglycemia acts as a major metabolic stressor. When your glucose drops below normal ranges, your body interprets it as an emergency and initiates a stress response to quickly elevate levels. This internal stress cascade can lead to fatigue, anxiety, brain fog, and headaches.
Go Beyond Glucose Data with Nutrisense
Your glucose can significantly impact how your body feels and functions. That’s why stable levels are an important factor in supporting overall wellbeing. But viewing glucose isn't enough. Nutrisense, you’ll be able to learn how to use your body's data to make informed lifestyle choices that support healthy living.
One-to-one coaching
Sign up to access insurance-covered video calls to work with a glucose expert: a personal registered dietitian or certified nutritionist who will help tailor your lifestyle and diet to your goals.
Monitor and measure what matters
With the Nutrisense CGM Program, you can monitor your glucose with health tech like glucose biosensors and continuous glucose monitor (CGM)s, and analyze the trends over time with the Nutrisense App. This will help you make the most informed choices about the foods you consume and their impact on your health.
Find your best fit
Ready to take the first step? Start with our quiz to find the right Nutrisense program to help you take control.
Go Beyond Glucose Data with Nutrisense
Your glucose can significantly impact how your body feels and functions. That’s why stable levels are an important factor in supporting overall wellbeing. But viewing glucose isn't enough. With Nutrisense, you’ll be able to learn how to use your body's data to make informed lifestyle choices that support healthy living.
Review Your Patterns Together
Sign up to access insurance-covered video calls with a glucose expert: a personal registered dietitian or certified nutritionist who will help tailor your lifestyle and diet to your goals.
Turn App Insights Into Action
With the Nutrisense program, you can monitor your glucose with health tech like glucose biosensors and continuous glucose monitors (CGMs), and analyze the trends over time with the Nutrisense App. This will help you make the most informed choices about the foods you consume and their impact on your health.
Take the First Step
Start with our quiz to find the right Nutrisense program to help you take control.

Kara Collier is a registered dietitian nutritionist and certified nutrition support clinician who is passionate about reshaping how we approach prevention, behavior change, and metabolic health. A Forbes 30 Under 30 honoree, she’s helped over 150,000 people improve their metabolic health using tools like continuous glucose monitors and behavior-focused nutrition strategies. Kara has been featured by Forbes, UC Berkeley, and HLTH, and has appeared on top podcasts like Mind Pump and The Genius Life.




