What Causes High Glucose? Symptoms and Management
Key Takeaways
- High glucose: This metabolic state occurs when there is more sugar circulating in your bloodstream than your body can efficiently use or store.
- High glucose causes: Elevated levels are often driven by highly processed diets, chronic stress, poor sleep patterns, or conditions like insulin resistance.
- Blood test meaning: A high glucose reading in a blood test typically means your fasting levels are over 100 mg/dL, which can indicate impaired metabolic function.
- High glucose: This metabolic state occurs when there is more sugar circulating in your bloodstream than your body can efficiently use or store.
- High glucose causes: Elevated levels are often driven by highly processed diets, chronic stress, poor sleep patterns, or conditions like insulin resistance.
- Blood test meaning: A high glucose reading in a blood test typically means your fasting levels are over 100 mg/dL, which can indicate impaired metabolic function.
Blood sugar naturally rises and falls throughout your day; that’s how your body keeps energy moving. Those shifts depend on what you eat, how you sleep, your stress, and even the time of day. So, some variation is normal.
But when this blood sugar, or glucose, stays higher than usual or spikes often, it’s worth paying attention. Those patterns can signal that your body is having a harder time keeping balance. Learning what’s behind them (and what your symptoms mean) can help you take small, specific steps toward better long-term metabolic health.
What does it mean to “have high glucose”?
To fully understand your blood glucose levels, it’s important to know what values are actually considered high, and which factors can cause your elevated readings in the first place.
Hyperglycemia vs hypoglycemia
High glucose, called hyperglycemia, means there’s more sugar circulating in your blood than your body can use or store.. Low blood sugar, or hypoglycemia, is the result of too little glucose in the bloodstream. Hyperglycemia usually occurs because your body doesn’t produce enough insulin or can’t properly use the available insulin to remove the glucose from the bloodstream.
In lab terms, post-meal readings between 140–199 mg/dL suggest prediabetes, while 200 mg/dL or more may point to diabetes (your doctor confirms this). Of course, it’s always best to do a few things:
- Go through labs, glucose readings, and symptoms with a glucose expert, like a trained registered dietitian.
- Work with your doctor before reaching any conclusions about insulin resistance or diabetes.
Common glucose ranges
A range of lifestyle factors, habits, and health conditions can cause high glucose. To debunk common hyperglycemia myths, review causes and symptoms, and discuss the best ways to address them, we spoke with two experts on high glucose levels: registered dietitian and For The Love of Diabetes creator Lori Zanini and registered dietitian nutritionist and diabetes management expert Mary Ellen Phipps.
Common high glucose myths
There are a handful of misconceptions surrounding high glucose. Some you might have heard before, some you may not even know are myths.
Myth: “Only people with diabetes get high glucose”
Even without diabetes, stress, sleep loss, or certain foods can raise glucose temporarily. When researchers studied people wearing a continuous glucose monitor who did not have a diabetes diagnosis, they found that glucose spikes are also associated with greater hunger and poorer mental health and sleep. Traditional glucose measurements, such as a single-point-in-time blood glucose value, are unable to capture these abnormalities.
There are actually several causes of high glucose unrelated to diabetes that the CDC recognizes. These include certain foods, like artificial sweeteners and coffee. Other factors, like stress, can do it, too. If you live with an endocrine or pancreatic condition, have had surgery recently, or are experiencing intense physical stress (say, from a sunburn), you may also see your glucose value rise.
Myth: “All carbs are created equal”
Phipps explains that, despite containing similar amounts of carbohydrates, one serving of pasta could have a hugely different effect on your blood glucose levels than one serving of rice. Likewise, that serving of pasta may have an entirely different effect on your blood glucose levels than your friends’ or even family members’. “We’re all unique,” Phipps says.

Myth: “If I feel fine, my glucose must be fine.”
High glucose can develop quietly; fatigue, thirst, or brain fog can be easy to dismiss until they persist.
Zanini points out that having high glucose can come as a surprise to anyone. “It's possible they didn't notice any symptoms or were simply feeling 'more tired than usual,’" she says. “It's easy to attribute being tired to many other things . . . this is why regular physicals with your healthcare provider are important.” The bottom line? Listen to your body, take note of symptoms as they arise, and consider monitoring your continuous glucose values.
Myth: “You can’t prevent high glucose”
According to the CDC, managing stress, staying active, and maintaining a balanced diet of fiber, protein, and fat can help prevent the development of type 2 diabetes. You can also work with your doctor and a registered dietitian to devise a routine that's both preventative and sustainable.
Myth: “If my A1C is normal, my glucose is good”
A1C shows a three-month average, but it can hide daily spikes and dips. An A1C result that’s below 5.7% is normal by the CDC’s standards, but having a result below that number isn’t the end of the story. Pregnancy, hemoglobin variants, anemia, liver disease, and certain medications can cause inaccurate A1C results.
Additionally, the A1C test measures your average glucose value over the past 3 months, but averages inherently do not capture highs and lows. So, you could have a normal average while also having abnormal glucose spikes. The A1C test should supplement, not replace, your regular blood sugar and glucose testing.
Is having high glucose dangerous?
In short, it can be. Registered dietitian Lori Zanini says that untreated high glucose can lead to a wide range of health issues—some of the most common being chronic inflammation, heart disease, vision impairment, kidney disease, nerve damage, tooth decay, damaged blood vessels, and periodontal disease.
Having high glucose also puts us at risk of mitochondrial dysfunction and oxidative stress. The former is a condition in which mitochondria fail to produce energy for cells. The latter occurs when free radicals outnumber antioxidants in the body, increasing the risk of disease and other damage.
Phipps notes that to avoid these risks, catching high glucose levels early and taking action to treat them is extremely important.
What causes high glucose?
Experts are still learning about the factors that can contribute to high glucose levels. With that in mind, these are the main known causes of high glucose.
Looking into that surprising lab result
You leave your annual physical feeling a little deflated. You exercise regularly and try to make smart food choices, but your doctor just told you your A1C is 5.8 percent, putting you in the prediabetic range. It’s confusing and frustrating.
You thought you were doing everything right, but the lab report says otherwise. Now you’re questioning every meal and wondering why the fatigue you’ve been brushing off might be something more. Don’t worry! Working with a registered dietitian, you can figure out what’s actually going on underneath the surface.
Causes related to personal health
These are factors inside your body. They can change insulin sensitivity, hormone balance, and how organs handle glucose. Work with your clinician to identify what applies to you so you can target the right levers.
Insulin resistance
Insulin resistance happens when your cells don’t respond as well to insulin, so glucose builds up in your blood instead of being used for energy.
Your pancreas responds to this increase in glucose by producing more insulin to help your body process it. This excess insulin in the bloodstream can eventually cause your body to lose insulin sensitivity or develop resistance to it, leading to higher blood glucose levels.
Body composition
Higher body fat, especially around the abdomen, is linked with elevated glucose and reduced insulin sensitivity.
In fact, a high body fat percentage might be a clearer indicator of high glucose and diabetes than weight or body mass index (BMI).

Other health conditions
Certain conditions may make you more likely to have high glucose levels. These include Cushing’s disease, polycystic ovarian syndrome (PCOS), and gestational diabetes. Blood glucose may also rise due to common illnesses such as a head cold or the flu.
Hormonal changes
It isn’t just stress and sleep that can cause fluctuations in hormones. Illness, physical pain and trauma, menopause, or menstruation can as well. In any of these instances, your blood glucose levels may rise due to the changes in your hormone levels.
Medications
Certain medications, including steroids and beta-blockers, can disrupt insulin’s effectiveness. Others, like second-generation antipsychotics and certain antibiotics, may contribute to high glucose. However, research to learn why this happens is ongoing.
Gut issues
A growing body of research links imbalances in the microbiota in our guts to an inability to regulate glucose levels. This is sometimes due to antibiotic use or infection.
Genetics
A family history of high glucose and specific genes may increase a person’s chances of having high glucose and developing diabetes. People with African American, American Indian, Asian American, Pacific Islander, or Hispanic heritage may face greater risks.
Causes related to your diet

What and how you eat shapes your glucose curve. Meal timing, portions, fiber, protein, fat, hydration, and micronutrients all influence how high and how long glucose rises. Responses are individual, so test and adjust.
Processed foods and refined sugar
Packaged or processed foods high in refined grains or added sugars can cause sharper, longer glucose spikes than whole foods.
Overeating or grazing
It’s a common belief that snacking throughout the day (a.k.a. “grazing”) will keep blood glucose levels steady. But research suggests that eating three or more meals a day may support better insulin sensitivity compared to eating fewer than three. It’s also important to keep our meals in the right proportions, as overeating can raise blood glucose levels.
Dehydration
Some research has found a connection between low water intake and a greater risk of hyperglycemia. This is most likely because less water in the body means the blood's glucose concentration is higher.
Vitamin and mineral deficiencies
Research into this cause is ongoing. Yet studies suggest that diets lacking micronutrients such as chromium, magnesium, or vitamin D may contribute to elevated glucose levels.
Causes related to your lifestyle
Daily habits set your baseline. Movement, stress, and sleep each affect insulin sensitivity and cortisol, which in turn affect glucose. Small, consistent changes here can meaningfully reduce spikes over time.
Physical inactivity
Exercising prompts your body to burn more energy than usual, and, as a result, consume more glucose. Maintaining a low level of physical activity, on the other hand, means more glucose will remain in the bloodstream. This raises your overall blood glucose values in the process.
Exercise also makes our bodies more insulin sensitive, which means we will require less insulin for the rest of the day to control glucose levels.
Stress

Part of the body’s fight-or-flight response to stress is to produce additional glucose. Another facet of that response is an increase in the hormone cortisol. High cortisol can reduce the body’s sensitivity to insulin. As a result, blood glucose levels may also increase.
Poor sleep
A lack of quality sleep can reduce the amount of insulin your body releases. It can also stimulate cortisol production, making it harder for insulin to work. When your body’s insulin cannot properly metabolize the glucose in your blood, the glucose remains there, and your glucose levels rise.
What are the main symptoms of high glucose?
While an individual may have no noticeable symptoms and still have high glucose, knowing which symptoms tend to accompany high glucose, such as frequent urination or brain fog, can help you take the right action before things get worse.
Fatigue and sleepiness
For example, if you've ever wondered whether high glucose can make you sleepy, the answer is yes. High glucose levels can contribute to feelings of fatigue and sleepiness. When there is excess glucose in the bloodstream, the body may struggle to effectively use it for energy. This can lead to a sense of lethargy and drowsiness.
Other common symptoms of hyperglycemia to be aware of are:
- Thirst
- Frequent urination
- Blurry vision
- Headaches and brain fog
- Increased cravings for carbs and sweets
- “Hanger”
- Poor energy levels or midday crashes
- Fatigue
- Unintentional weight loss
- Slow-healing cuts
How is high glucose diagnosed
Doctors use four main tests to gauge patients’ blood glucose levels:
1) Fasting glucose test
Conducted after fasting for eight hours, a reading of 100 mg/dL or more is considered high or a sign of prediabetes, while a reading of at least 126 mg/dL indicates type 2 diabetes. However, for optimal health, we recommend aiming for a fasting glucose value below 90 mg/dL.
2) Oral glucose tolerance test
Conducted after fasting for eight hours, drinking a high-sugar glucose solution, and waiting two more hours, a reading of at least 140 mg/dL is considered a sign of prediabetes. A reading of 200 mg/dL or higher is type 2 diabetes. For optimal health, aim for a two-hour glucose of 110 mg/dL or lower.
3) Random glucose test
Conducted at any time throughout the day, a reading of at least 200 mg/dL indicates type 2 diabetes.
4) A1C test
Conducted at any time throughout the day, a result below 5.7% is considered normal. A result greater than 5.7% is considered an indication of prediabetes, and a result of 6.5% or higher indicates type 2 diabetes.
Find the right Nutrisense programto turn insight into progress.
See what’s really behind your glucose highs
See what’s really behind your glucose highs
How can you lower high glucose
Zanini says high-glucose treatment is a highly individualized process based on several personal details. These include age, pre-existing conditions, current medications, and current blood glucose value. But several overarching lifestyle changes can help reduce high glucose.
Address a poor diet

Everyone can benefit from consuming a diet rich in whole foods. It’s further beneficial to minimize intake of processed foods, such as foods containing sugar, flour, and vegetable seed oil. While there is no “best” diet for everyone, this golden rule of nutrition can help any person get more from their meals.
Personalized nutrition makes room for your unique differences and takes your individuality into account. The best way to find your perfect diet is to test different approaches, experiment, work with a dietitian, and use data, such as glucose monitoring, to assess whether something is working.
Maintain an active lifestyle
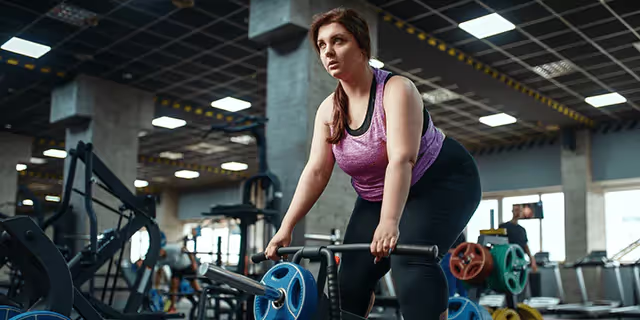
Take breaks during a sedentary workday, add a walk around the block to your morning routine, or try a new form of exercise. These activities bring great benefit in both the short and long term while helping reduce your overall stress. Including regular strength training and aerobic exercise will also help lower glucose levels.
Manage stress
Make stress-relieving practices, such as reframing your thoughts and soothing breathing exercises, part of your daily routine. Doing so will reduce your overall stress and, in turn, help prevent cortisol spikes.
Get adequate sleep
Getting good rest will help regulate your hormones and reduce unwanted spikes in your blood glucose levels.
Maintain a healthy weight
According to the Centers for Disease Control and Prevention (CDC), maintaining a healthy weight can help reduce your risk of developing high glucose and diabetes. If you’re working toward a healthy weight, the ADA recommends creating a sustainable routine you can stick with and focusing your efforts toward realistic goals.
Take medication as prescribed by your doctor
A doctor may prescribe antidiabetic medication, such as metformin, to help lower your blood glucose levels. If you’re at high risk of developing diabetes, taking this medication is crucial for lowering high glucose levels.

When should you see a doctor?
Your yearly doctor’s appointment is an excellent time to check in on your blood glucose levels. This is especially true if your age (over 45 years old), weight, or family history puts you at higher risk for developing diabetes in general.
Emergency symptoms
If you suspect you may already have high glucose, Zanini says that any changes in your health are a reason to see your doctor. Make an appointment to undergo the diagnostic tests listed above and to discuss treatment options with your provider.
If you have high glucose and experience trouble breathing, vomiting, confusion, extremely high thirst, or other symptoms of diabetic ketoacidosis, seek medical attention right away. This condition occurs when your body burns fat too quickly, producing ketones that make your blood acidic. It can be life-threatening if left untreated.
DKA and HHS: Emergency warning signs and when to test ketones
DKA and HHS are hyperglycemic emergencies. Learn the warning signs and when to test ketones so you can act fast. See the ADA and EASD 2024 consensus for clinical details.
- Check urine or blood ketones during illness or when very high readings persist, especially in individuals with type 1 diabetes or during an infection. Seek urgent care if ketones are positive or if symptoms below appear.
- If you use a continuous monitor, remember it reports glucose measured in interstitial fluid. Follow your clinician’s guidance if symptoms are concerning.
- DKA warning signs include nausea or vomiting, abdominal pain, deep or rapid breathing, fruity breath, dehydration, fatigue, and confusion.
- HHS red flags include very high readings, often 600 mg/dL or higher, extreme thirst and dry mouth, frequent urination, severe dehydration, drowsiness, or confusion.
- Call your clinician or emergency services if you have positive ketones, persistent marked hyperglycemia with symptoms, or any DKA or HHS warning signs.
How can you tell if your glucose is high
When learning more about your overall health and how your body responds to your routines, staying informed about your blood glucose levels should be a top priority. The following glucose monitoring options can help you get a better picture of your health:
Blood tests
As previously described, your doctor can conduct a series of blood tests to determine your blood glucose level. These may include a fasting or random blood glucose test.
Oral Glucose Tolerance Test
Your doctor may also conduct an oral glucose tolerance test. This procedure requires you to fast for eight hours, drink a high-sugar solution, and wait two more hours before your doctor tests your blood. From that test, they can identify your blood glucose level.
Glucometer
Also known as a glucose meter, this device tests your blood glucose level with a finger prick. It can provide you with on-demand readings of your blood glucose levels.
Continuous glucose monitors (CGM) or glucose biosensors
Wearables and health tech like glucose biosensors and CGMs have a wealth of benefits. They measure your levels through a small, painless device on the back of your arm, keeping you updated on your glucose 24/7 and showing your responses to food, exercise, and other routines in real time.
Prioritizing sleep, nutrition, and regular doctor’s visits are key to maintaining a healthy glucose level. They're also highly effective preventative measures. Keeping track of new symptoms or changes in your health, like weight loss, fatigue, or increased thirst and urination, is also important.
How can Nutrisense support your goals
Your glucose can significantly impact how your body feels and functions. That’s why stable levels are an important factor in supporting overall well-being. But viewing glucose isn't enough. With Nutrisense, you’ll learn how to use your body's data to make informed lifestyle choices that support healthy living.
Sign up to access insurance-covered video calls with a glucose expert: a personal registered dietitian or certified nutritionist who will help tailor your lifestyle and diet to your goals.
Track with the app
With the Nutrisense Program, you can monitor your glucose using health tech like glucose biosensors and continuous glucose monitors (CGMs), and analyze trends over time in the Nutrisense App. This will help you make the most informed choices about the foods you consume and their impact on your health.
Start with our quiz
Ready to take the first step? Take our quiz to find the right Nutrisense program to help you take control.
Frequently Asked Questions
What causes high glucose?
High glucose is caused by a combination of dietary choices, lifestyle factors, and metabolic conditions. Consuming excess carbohydrates, experiencing chronic stress, or having poor sleep can all drive elevated levels. Tracking your individual glucose response can help pinpoint your specific triggers.
Does high glucose make you sleepy?
Yes, high glucose can cause fatigue and sleepiness. When your body cannot efficiently move glucose from the bloodstream into your cells, your energy levels drop. This mechanism explains why many people feel sluggish after a carbohydrate-heavy meal.
What causes fasting glucose to be high?
High fasting glucose is often caused by the dawn phenomenon or poor sleep quality. Your body naturally releases hormones in the early morning that temporarily raise glucose to provide waking energy. If you have underlying insulin resistance, your body may struggle to balance this natural morning surge.
Go Beyond Glucose Data with Nutrisense
Your glucose can significantly impact how your body feels and functions. That’s why stable levels are an important factor in supporting overall wellbeing. But viewing glucose isn't enough. Nutrisense, you’ll be able to learn how to use your body's data to make informed lifestyle choices that support healthy living.
One-to-one coaching
Sign up to access insurance-covered video calls to work with a glucose expert: a personal registered dietitian or certified nutritionist who will help tailor your lifestyle and diet to your goals.
Monitor and measure what matters
With the Nutrisense CGM Program, you can monitor your glucose with health tech like glucose biosensors and continuous glucose monitor (CGM)s, and analyze the trends over time with the Nutrisense App. This will help you make the most informed choices about the foods you consume and their impact on your health.
Find your best fit
Ready to take the first step? Start with our quiz to find the right Nutrisense program to help you take control.

Kara Collier is a registered dietitian nutritionist and certified nutrition support clinician who is passionate about reshaping how we approach prevention, behavior change, and metabolic health. A Forbes 30 Under 30 honoree, she’s helped over 150,000 people improve their metabolic health using tools like continuous glucose monitors and behavior-focused nutrition strategies. Kara has been featured by Forbes, UC Berkeley, and HLTH, and has appeared on top podcasts like Mind Pump and The Genius Life.