How to Lower A1C Levels: 9 Diet and Lifestyle Strategies

Key Takeaways
- Carbohydrate pairing: Consuming carbohydrates on their own can lead to rapid glucose spikes, but pairing them with protein, fiber, and healthy fats helps blunt this response and supports lower average levels over time.
- Meal sequencing: Eating your healthy fats, protein, and non-starchy vegetables before consuming any carbohydrates can further reduce glucose swings and improve your A1C.
- Weight loss impact: Losing 5 to 10 percent of your total body weight can significantly improve your A1C, and managing it at a safe rate of one to two pounds per week offers the most sustainable results.
- Carbohydrate pairing: Consuming carbohydrates on their own can lead to rapid glucose spikes, but pairing them with protein, fiber, and healthy fats helps blunt this response and supports lower average levels over time.
- Meal sequencing: Eating your healthy fats, protein, and non-starchy vegetables before consuming any carbohydrates can further reduce glucose swings and improve your A1C.
- Weight loss impact: Losing 5 to 10 percent of your total body weight can significantly improve your A1C, and managing it at a safe rate of one to two pounds per week offers the most sustainable results.
Start by Taking an A1C Test
You may have heard of A1C tests as hemoglobin A1C, glycosylated hemoglobin, HbA1c, or estimated average glucose (eAG) tests. They're a tool to screen for pre-diabetes, diagnose diabetes, or monitor a diabetes treatment plan.
The A1C test measures the percent of hemoglobin proteins in the blood coated with sugar. It also reflects average blood sugar (glucose) levels for the past two to three months. There are some flaws with this test, though. So, we also want to consider blood glucose readings, the frequency of highs and lows on these readings, and your lifestyle. For more on A1C testing, check out this article!
Does everyone need an A1C test? It depends on several factors, such as your age and medical history. People over 45 and those under 45 with risk factors for pre-diabetes or diabetes should. If the results are normal, both groups should take the test annually or according to their primary doctor’s recommendations. Those with pre-diabetes should consider having their A1C assessed more frequently.
The frequency of an A1C test for those with diabetes depends on their self-management. Someone who is not on insulin, who has blood glucose values within their target range, should take the test twice a year. People on insulin or those who have trouble keeping their blood glucose stable can get quarterly tests. As we already know, the A1C test looks at your average blood glucose values for two to three months. So, you don’t need to take it more than once every three months.
What’s Considered a High A1C Level and Is It Possible to Lower It?
People with higher blood sugar values have more sugar attached to their hemoglobin, which leads to a higher A1C. It's important to speak with your doctor about your specific A1C goals. But if you're curious, here's what those numbers on your results mean:
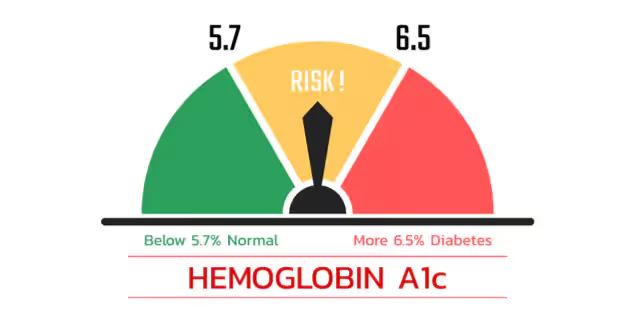
As you can see from the image, a 'normal' range is <5.7%, 5.7-6.5% is seen as a risk of pre-diabetes, and >6.5% reads as diabetes.
Even though <5.7% is considered ‘normal,’ some compelling research suggests that a lower A1C aligns with appropriate glucose tolerance more accurately. Some studies have suggested aiming for an A1C around 5.3%, but researchers are still determining the optimal value.
It's common for those diagnosed with type 2 diabetes to aim for an A1C of 7% or less.
Seeing elevated A1C levels can be distressing, and it could leave you wondering if it's possible to lower them. Fortunately for you, the answer is yes! This isn't a quick fix, though, since the amount of time it takes to see any improvements can vary.
If your A1C levels were initially high (think close to 10%), they'll likely come down quicker with diet and lifestyle changes. If your levels were only moderately elevated, it might actually take longer for them to come back down with those same changes. Remember that the test looks at average blood sugar values over two to three months, so you can expect it to take at least that long to see any improvement.
9 Ways to Lower Your Hemoglobin A1C Levels

1. Eat More Protein, Non-Starchy Vegetables, and Healthy Fats
When we eat carbohydrates on their own, our body quickly and easily breaks them down to glucose that it then uses for energy. This can contribute to glucose spikes, and ultimately, to higher A1C levels.
But don't swear off carbohydrates just yet—there's another way to avoid these spikes. Instead, pair protein, fiber (like non-starchy vegetables), and healthy fats with your carbohydrates. This blunts the glucose response and helps you achieve more stable, less extreme glucose values. Over time, this will also lead to lower A1C levels.
A good rule of thumb to follow for great blood sugar control is eating more low-carb vegetables, protein, and healthy fats, along with a moderate serving size of carbohydrates. You can mix and match based on your preferences and lifestyle, but here are some options to help you start out:
- Add some vegetables: There’s so much to pick from. Try broccoli, cauliflower, Brussels sprouts, celery, and asparagus. Or, consider cucumber, kale, peppers, spinach, tomatoes, cabbage, zucchini, mushrooms, and onions. You can eat these raw, roasted, boiled, steamed, or lightly sautéed.
- Pick a protein: Good options include chicken, beef, tofu, fish/seafood, organ meat, eggs, pork, turkey, and duck.
- Find a healthy fat: Think avocados, olives, unrefined vegetable oils (coconut, olive, avocado), butter, and pesto.
Since we're most sensitive to carbs on an empty stomach, the order in which we eat can also affect our glucose. One way to ensure steadier glucose levels is to try meal sequencing. This involves a solid base of healthy fats, protein, or fiber before you eat any carbohydrates. It will help reduce glucose swings.
2. Plan Your Meals

Planning meals can enable you to hold yourself accountable and stick to your goals. A set schedule for daily meals can also help you avoid making poor eating decisions when hungry and time-crunched. Of course, this doesn't mean that you have to plan every meal, snack, and beverage you consume down to the minute (unless that's what works for you!). But having a rough idea of how you'd like to eat can be helpful.
Be realistic about your schedule and how much time you have for meal preparation. For some people, two to three-day plans are more manageable. For others, planning for the week ahead works best. When you know you have a busy day ahead, focus on meals that you can throw together in a pinch. Or, consider doing some prep work, like chopping vegetables and marinating meats, the night before.
Don't forget to stay flexible so you can plan for emergencies and last-minute disruptions in your schedule. Having a few grab-and-go items in your pantry can make hectic days easier to manage. Some helpful options include rotisserie chicken, bagged salads, hard-boiled eggs, frozen or pre-chopped vegetables, and pre-cooked shrimp. You can add these items to salads and soups or combine them with other ingredients for a simple yet satisfying meal.
3. Measure Everything—Portion Sizes to Tracking Carbs
Can you tell how many grams of carbohydrates you're consuming just from looking at an apple (if you’re curious, a medium apple has around 25g)? Not many of us possess that skill, which is why it's easy to underestimate how many carbohydrates you're actually eating.
Using a food tracking app can help you learn about appropriate serving sizes and give you an idea of your total carbohydrate intake in a day. This can also help you stay accountable and stick to your goals.
4. Set a Weight Loss Goal
Losing 5-10% of your body weight can improve A1C, so if you're overweight, you may want to consider using that percentage as your weight loss goal. If you're on medications for diabetes, you may find that you need less medication as you lose weight.
The key to weight loss that will actually work is to set a realistic goal with a sustainable weight loss target. A safe bet is 1-2 pounds per week, so if you know that you want to lose 20 pounds, plan on spending two and a half to three months working at it. Using a continuous glucose monitor (CGM) can help you develop a personalized plan for weight loss.
5. Work With a Dietitian
Not sure where to start when it comes to planning meals or choosing foods to help lower your A1C? Working with a dietitian can help! There are many conflicting nutrition recommendations. It can be a challenge to sort through them all and pick the perfect one for your individual needs.
A registered dietitian can help you wade through the options to find the right program for you. They often look at your medical history, preferences, and lifestyle to tailor it to your needs. It's important to pick a dietitian you can be open and honest with. So, take the time to find a dietitian that you can trust to help you on this journey.
6. Have an Exercise Plan

The American Diabetes Association recommends getting 150 minutes of moderate-intensity exercise per week. This stems from the fact that all types of exercise improve insulin sensitivity and glucose control. This can also ultimately help with your A1C levels.
Exercise plans, much like meal plans, encourage you to stick to your goals. Here are some tips that may help you plan your new exercise regime:
- Choose an exercise you enjoy: If you hate using the elliptical, your chances of sticking with it are low. If you love it, you'll look forward to it, even start to miss it on days you don't work out. Pick something you love—it's okay if this takes a little trial and error.
- Start slow: If you jump right into an exercise regime, especially without a trainer, there's a good chance you'll end up injuring yourself. It can be challenging to wait for tangible results, but going slow can help you build on your progress instead of jeopardizing it.
- Reorganize your schedule: Want to work out first thing in the morning? Prefer to exercise after a long day at work? Pick a time that works best for your unique lifestyle. If you fold it into a routine that already works for you, you have a better chance of sticking to it.
- Set SMART goals: SMART stands for specific, measurable, attainable, realistic, and time-based. Setting goals with this in mind will help with accountability. Try something concrete and attainable, like "I will do yoga 3 days/week for 20 to 30 minutes, all of next month," instead of "I will do yoga every day next month."
- Find a workout buddy: Finding it hard to hold yourself accountable? Just ask someone else to do it for you! A workout buddy is a win-win situation for both parties. If you're the sort of person who works better amidst company, it can make your workouts more enjoyable too.
- Track your progress: Logging your workouts can help you feel a sense of accomplishment that can keep you motivated.
- Diversify your workouts: Bored with the elliptical you once loved? Try yoga! Tired of running on the treadmill every day? Consider running outdoors. Switching things up once in a while can keep things fresh and help you stay motivated.
7. Manage Your Stress and Mental Health
Did you know that stress can impact your glucose? Our bodies have a fight or flight response to stress. This increases glucose production and reduces insulin sensitivity, leading to higher glucose.
Just like getting started with exercise, learning to manage stress can take some time and practice. Here are a few techniques to consider:
- Pick a breathing technique: Breathing exercises are some of the easiest ways to manage stress and often the simplest. Try timeworn techniques like deep belly breathing or the 4-7-8 breathing exercise.
- Try meditation: Try using an app to help you begin, like Simple Habit, Headspace, or Calm.
- Stick to a routine: A routine, or a set of daily habits, can help remove some of the anxiety and stress that comes with the uncertainty of life. Maintaining a hobby, spending time with loved ones, even just reading a particular blog every day—it can all alleviate stress.
- Block nighttime blue light: Blue light, especially at nighttime, disrupts your circadian rhythm. To avoid this, stay away from screens a few hours before bedtime. Also, consider wearing blue-light-blocking glasses when you do use them.
You can't avoid stress altogether, but these techniques, coupled with adequate sleep (more on that below!), can help you manage it. Taking care of your mental health is also essential when you're trying to manage stress. So don't hesitate to seek professional support if you need to.
8. Get the Right Amount of Sleep
The role sleep plays when it comes to optimizing A1C is interesting. If you don't already know, sleep and glucose values have what's known as a bidirectional relationship. This means higher glucose can lead to a worse night of sleep and that poor sleep can cause suboptimal glucose the next day.
A study from 2019 looked at sleep duration and A1C levels in 962 individuals with either pre-diabetes or untreated type 2 diabetes. They found that those who slept a consistent seven to eight hours every night had significantly better A1C values than those who slept either five hours or less or more than eight hours.
Consider incorporating healthy sleep hygiene habits to get better sleep and optimize your A1C in the process, like:
- Set a routine: As mentioned above, it's important to have a routine. Not only does it help with stress, but it's also directly related to your A1C levels. So, try to go to bed and wake up at the same time every day.
- Create a sleep space: It's just as important to have a space that encourages good sleep as it is to get to bed. Leave the electronics out, keep your bedroom cool and dark, and find a bedtime routine that allows your body to relax.
- Cut out caffeine: A little caffeine is unlikely to cause a spike among most people. According to the Mayo Clinic, a safe amount for a healthy adult is up to 400 milligrams per day. Too much can lead to high A1C levels, though, so minimize your intake, particularly later in the day.
- Get some sun: Sunlight helps to regulate your circadian rhythm and sleep better at night. Getting 30 minutes of sunlight, especially in the morning, can help jumpstart your day.
9. Try Some Berberine
Berberine is an herbal compound that may help improve glucose levels. It's often explored as a possible therapy in diabetes, but the specifics of how it works to help glucose levels are not entirely clear.
It's thought to work either by increasing insulin receptor activity (making it easier for glucose to leave the bloodstream and enter our cells) or through its antimicrobial effects. As with any supplement, this could interfere with some medications, so discuss with your doctor before trying.
Find the right Nutrisense programto turn insight into progress.
Frequently Asked Questions
Is a 5.3 A1C considered prediabetes?
No, a 5.3% A1C is not considered prediabetes. The risk range for prediabetes typically begins at 5.7%. If your reading is 5.3%, it falls within the normal range and does not indicate a prediabetic state.
What does an A1C of 5.3 mean?
An A1C of 5.3% means your average blood glucose has been in a healthy range over the past two to three months. While anything under 5.7% is considered normal, some research suggests that a 5.3% value may actually be the optimal target for appropriate glucose tolerance.
Can you lower your A1C in a month?
It is unlikely to see significant A1C improvements in just one month. Because this test measures the percentage of sugar-coated hemoglobin proteins over a two to three-month period, you generally need to maintain new diet and lifestyle habits for at least 90 days before they reflect on your results.
Go Beyond Glucose Data with Nutrisense
Your glucose can significantly impact how your body feels and functions. That’s why stable levels are an important factor in supporting overall wellbeing. But viewing glucose isn't enough. Nutrisense, you’ll be able to learn how to use your body's data to make informed lifestyle choices that support healthy living.
One-to-one coaching
Sign up to access insurance-covered video calls to work with a glucose expert: a personal registered dietitian or certified nutritionist who will help tailor your lifestyle and diet to your goals.
Monitor and measure what matters
With the Nutrisense CGM Program, you can monitor your glucose with health tech like glucose biosensors and continuous glucose monitor (CGM)s, and analyze the trends over time with the Nutrisense App. This will help you make the most informed choices about the foods you consume and their impact on your health.
Find your best fit
Ready to take the first step? Start with our quiz to find the right Nutrisense program to help you take control.
Kara Collier is a registered dietitian nutritionist and certified nutrition support clinician who is passionate about reshaping how we approach prevention, behavior change, and metabolic health. A Forbes 30 Under 30 honoree, she’s helped over 150,000 people improve their metabolic health using tools like continuous glucose monitors and behavior-focused nutrition strategies. Kara has been featured by Forbes, UC Berkeley, and HLTH, and has appeared on top podcasts like Mind Pump and The Genius Life.