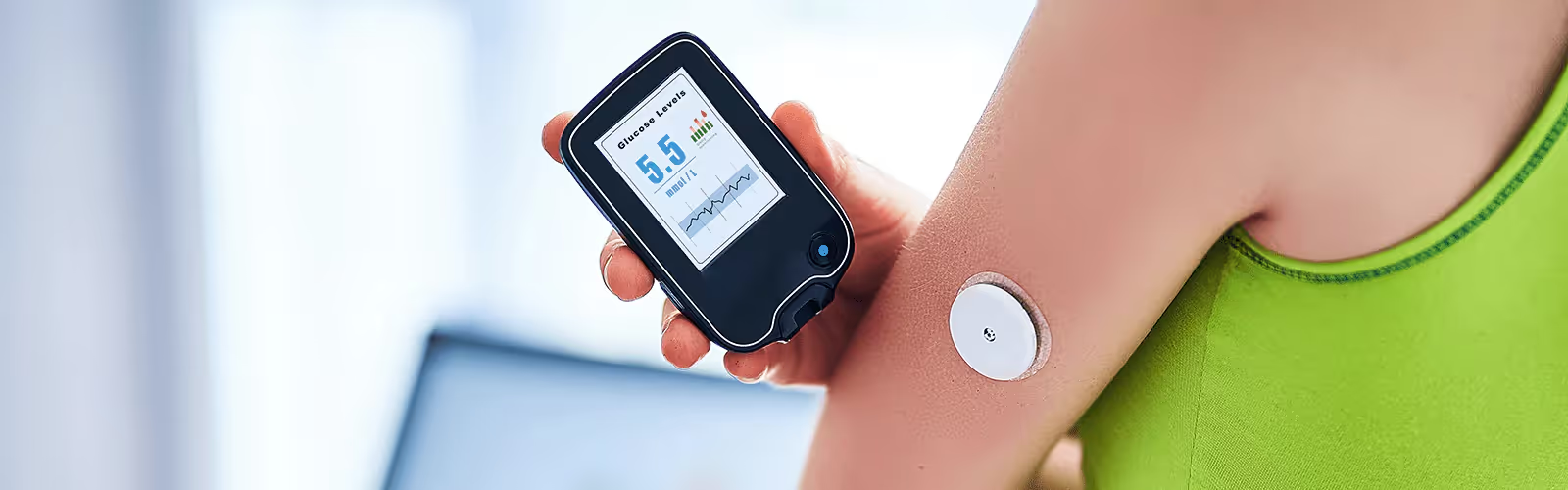
Blood Sugar Fluctuations: 17 Common Causes to Watch For
.avif)
Key Takeaways
- Blood sugar fluctuations: It is normal for your glucose levels to rise and fall throughout the day in response to daily habits, meals, hormones, and physical activity.
- Causes of erratic levels: Factors like lack of sleep, stress, extreme weather, and complex medications can trigger unpredictable swings in your individual glucose response.
- Fluctuation symptoms: Experiencing unstable glucose variability can lead to noticeable side effects like sudden fatigue, increased thirst, or difficulty sleeping, even without a diabetes diagnosis.
- Blood sugar fluctuations: It is normal for your glucose levels to rise and fall throughout the day in response to daily habits, meals, hormones, and physical activity.
- Causes of erratic levels: Factors like lack of sleep, stress, extreme weather, and complex medications can trigger unpredictable swings in your individual glucose response.
- Fluctuation symptoms: Experiencing unstable glucose variability can lead to noticeable side effects like sudden fatigue, increased thirst, or difficulty sleeping, even without a diabetes diagnosis.
Managing your blood sugar levels is essential when you're learning to live with diabetes. But having large swings in blood sugar can be harmful even if you don’t have a diabetes diagnosis.
Whether you’re making necessary lifestyle modifications or not, there are other things to consider with or without a diagnosis. After all, high glucose levels can sometimes be an indicator of a potential diabetes diagnosis. So, while watching what you eat is an effective way to control blood sugar, remember that there are various other factors that can also affect your glucose.
Keeping track of these is vital because ignoring them can potentially disrupt your efforts at managing your blood sugars. And even if you don’t have diabetes, your blood sugar still affects your sleep, how you feel throughout the day and may even determine how long you live.
Of course, how, what, and when you eat is still a core component when measuring your blood sugar. But to make managing blood sugar levels easier, here’s a list of some other causes of fluctuations to watch for:
1) Morning Hormone Levels (Dawn Phenomenon)

You’ve probably heard the phrase “body clock.” If you don’t already know, this means that with or without an alarm to coax you out of bed, you will usually wake up around the same time every morning (save for that late night out partying!).
This “dawn phenomenon” is the consequence of a measurable, chemical response within your body. In line with our diurnal lifestyles (in contrast to some animals’ nocturnal tendencies), the body produces certain hormones. These encourage you to wake up sometime after the sun rises to take advantage of all that beneficial daylight.
These sleep/wake cycles result from those hormones inciting your body to produce extra blood sugar, giving you a much-needed shot of energy to start the day. While this is a welcome evolutionary edge, it can sometimes come at the cost of skewing your blood glucose levels, at least temporarily. Check out our article on morning blood glucose to learn more about this phenomenon and other blood sugar quirks you might experience after waking up.
2) Your Hydration
It’s no secret drinking water is good for you. And human beings really are mostly water: the liquid portion of your blood (the plasma) is made of over 90 percent of water. With water’s tendency to dilute substances that it’s mixed into, the more water you drink, the more excess blood sugar is washed out of your blood through your urine and endocrine system. In contrast, the closer you are to dehydration, the more concentrated your blood sugar levels can become.
3) Extreme Weather Conditions
If dehydration can spike blood glucose, it’s no surprise that you should also be monitoring other conditions that cause water loss in your body. For example, you sweat when it’s hot, and when you sweat, you lose more water than usual. This can then put you at risk of blood sugar-related complications. An increase in glucose is often seen with heat exposure—this can be due to changes in fluid related to heat as well as stress responses to heat.

4) Sugar-free Foods
Particularly insidious is the effect of artificial sweeteners, often found in foods labeled as sugar-free (or “diet”), to provide a sweet kick without the guilt of natural sugar. It’s not yet clear why, but recent studies show that the body can react negatively to these sweeteners, paradoxically spiking blood sugar despite the absence of any actual sugar.
Further damning these sweeteners are their measured effect on insulin resistance. Your body can be tricked into treating artificial sweeteners similarly to sugar, producing excess insulin in response and building insulin resistance, a precursor to diabetes.
While sugar-free foods help you keep daily calorie counts low, manage diabetes, and maintain a healthy weight, it’s a good idea to eat foods containing artificial sweeteners in moderation.
5) Cold Medications
Artificial sweeteners find themselves included in much more than sugar-free foods. It’s worth the time it may take to read ingredient labels to see if sweeteners have made their way into anything you consume regularly. This can include over-the-counter medicines, which may contain artificial sweeteners to mask their bitter taste and make them more palatable. Depending on how your body responds to artificial sweeteners, it may be better to select a pill that’s harder to swallow but easier on your blood sugar levels.
6) Birth Control
Evolving research has shown associations between contraceptives that affect the hormones relevant to reproduction (like birth control pills, rings, implants, and patches) and blood sugar levels. If you’re pre-diabetic or have diabetes, it’s a good idea to speak with your doctor about what birth control is best for you.
7) Steroids
Medical conditions that demand taking anti-inflammatory medications may call for regular doses of steroids. No matter how they’re administered, many steroids are known to increase blood glucose levels. This is due to the hormones they encourage your body to release, causing your liver to subsequently release stored glucose.
8) Lack of Sleep

We’ve gone over the effects of sleep on blood sugar and vice versa. But here’s the most crucial role sleep plays in controlling blood sugar: the less consistent rest you get, the less your body can regulate the hormones it secretes.
Certain hormones in your body can change how it reacts to insulin. If you become more insulin resistant, you’re less able to naturally regulate your blood sugar levels. Taken to an extreme, this can spiral into a cycle of further increasing insulin resistance, causing less and less blood glucose regulation, ultimately leading to diabetes complications.
9) Caffeine Consumption

Besides potentially ruining a night of good sleep, caffeine may produce other measurable effects on blood sugar levels. Unfortunately, there’s no consensus on what factors are at play or whether diabetics are particularly sensitive to caffeine consumption. Remember, there’s no one-size-fits-all here! So, there’s no consensus yet on who might see their blood sugar levels drop, instead of rise, from caffeine intake. Your best bet is to experiment to see how your body responds to caffeine. As with any new additions to your diet and lifestyle, approach this cautiously and consider getting personalized advice from a doctor or dietitian.
10) Menstrual Cycles
The pattern of hormones and their relation to blood sugar fluctuations continues with another significant influence on hormonal balance. Like birth control, your menstrual cycle can spike your blood glucose levels through the body’s natural reaction to the increased levels of the specific hormones released.
Experts recommend caution when reacting to such spikes, so if you have diabetes and are on insulin, don’t go increasing your insulin in response. It may inadvertently leave you overly sensitive if your sugar levels return to normal more rapidly than you anticipate.
11) Alcohol Consumption
Drinking excessively is always a bad idea, but remember that even a moderate amount can affect your blood sugar levels. When alcohol is broken down, much of the glucose management occurs in your liver. Instead of occupying itself with releasing glucose promptly, your liver can become distracted with breaking down any alcohol recently consumed, potentially leading to a drop in your sugar levels. It’s a good idea to drink in moderation and monitor how alcohol reacts to your body when you do.
12) Exercise

Exercise is part of the foundation of a healthy lifestyle. It has even been found to reverse the onset of prediabetes. So it might seem unfair that you still have to be mindful of your blood sugar levels when exercising as part of your diabetes management plan.
The type and intensity of the exercise can play a role in whether your sugar levels rise or fall, but what may matter even more is if you’re exercising fasted or fed. If you’ve just eaten, your body has the energy to get through an exercise routine before your liver starts secreting more of its stored glucose to supplement it. At the end of the day, regular exercise has a net beneficial effect on your blood glucose, so there’s no reason to avoid it!
If you have diabetes or want to know more about how exercise impacts your glucose, speak with a health professional to develop a safe and effective exercise plan.
13) Stress
Your body naturally responds to the demands of any extra exertion by producing hormones to tell itself to release its stored energy. When that energy source is glucose, it spikes your blood sugar levels. The signal to release that energy is your fight-or-flight response. It doesn’t discriminate between exertion through regular exercise or through other sources of stress.
Humans developed this response as a way to exert a lot of energy really quickly if and when necessary. This is great if you’re being chased by a tiger but not always suitable for other sources of stress. Daily ups-and-downs and one-off instances of anxiety can trigger the same response, affecting your glucose levels in the same way.
14) Depression
Depression is a broad condition that can have elevated incidences among those with diabetes. Suffering from depression doesn’t necessarily affect your blood sugar on its own. Still, the correlations are well established and are likely consequential to how you react to a diabetes diagnosis. So, while stress and depression can affect everyone, managing diabetes can make everything more challenging.
15) Gut Health
Recent studies have shown promising correlations between your gut flora, the bacteria living within the gastrointestinal system, and secondary associations with your blood sugar. Certain bacteria (though it’s still uncertain which) can influence your liver to release its stored glucose.
While this is still being explored, remember that balanced diets (including recommended amounts of fiber, prebiotics, and probiotics) may help regulate and feed the bacteria in your gut. This may be able to ensure blood sugar control and a balance of the types of bacteria that live within you.

16) "Naked" Carbohydrates
High-carb foods are a guilty pleasure for all of us, so don’t worry too much about the occasional craving. But a diet that’s primarily filled with high-carb foods may be cause for concern. If you have diabetes or have been working with a glucose-certified dietitian or nutritionist you may already know the body breaks down carbohydrates into sugar. Naturally, more sugar will raise your blood sugar levels, so remember to monitor and moderate this.
Things get more complicated when it comes to complex carbohydrates. A complex carb is a carb whose molecular structure is more complicated than those associated with simple or “naked” carbs. For example, when you eat whole grains, where the carbohydrates remain molecularly unbroken, your body takes longer to disassemble the molecules into their simple constituent sugars.
In contrast, if you eat something that’s heavily milled and processed (like plain pasta or white bread), you may see a blood sugar spike in response to the carbs being so easily and rapidly broken down.
17) Altitude
High altitudes can put you at risk of both hypoglycemia and hyperglycemia. This doesn’t necessarily include air travel, where conditions are controlled to emulate surface conditions (though we still recommend speaking with your doctor before flying). If you have diabetes and you’re planning a high-altitude hike or a trip somewhere high above sea level, it’s a good idea to monitor your glucose levels.
Find the right Nutrisense programto turn insight into progress.
Frequently Asked Questions
Why does blood sugar go up and down?
Your glucose levels naturally rise and fall as your body processes energy. After you eat, carbohydrates are broken down into sugar, causing a spike, while exercise or fasting can lower those levels as the stored energy is used. Tracking your 24/7 data can help you understand these daily patterns.
What causes blood sugar to fluctuate?
Fluctuations are triggered by a mix of diet, lifestyle, and environmental factors. While meals are the most common cause, things like poor sleep, high stress, dehydration, and certain medications can also create unpredictable swings. A Registered Dietitian can help you identify which specific factors impact your metabolism the most.
What are the symptoms of blood sugar fluctuations?
Common signs include sudden changes in energy, frequent thirst, or unusual cravings. You might also experience brain fog, headaches, or disrupted sleep as your body struggles to maintain stable glucose. Monitoring your individual glucose response can help pinpoint the causes behind these daily symptoms.
Go Beyond Glucose Data with Nutrisense
Your glucose can significantly impact how your body feels and functions. That’s why stable levels are an important factor in supporting overall wellbeing. But viewing glucose isn't enough. Nutrisense, you’ll be able to learn how to use your body's data to make informed lifestyle choices that support healthy living.
One-to-one coaching
Sign up to access insurance-covered video calls to work with a glucose expert: a personal registered dietitian or certified nutritionist who will help tailor your lifestyle and diet to your goals.
Monitor and measure what matters
With the Nutrisense CGM Program, you can monitor your glucose with health tech like glucose biosensors and continuous glucose monitor (CGM)s, and analyze the trends over time with the Nutrisense App. This will help you make the most informed choices about the foods you consume and their impact on your health.
Find your best fit
Ready to take the first step? Start with our quiz to find the right Nutrisense program to help you take control.
Kara Collier is a registered dietitian nutritionist and certified nutrition support clinician who is passionate about reshaping how we approach prevention, behavior change, and metabolic health. A Forbes 30 Under 30 honoree, she’s helped over 150,000 people improve their metabolic health using tools like continuous glucose monitors and behavior-focused nutrition strategies. Kara has been featured by Forbes, UC Berkeley, and HLTH, and has appeared on top podcasts like Mind Pump and The Genius Life.