Why Is My Blood Sugar High in the Morning? Causes for Non-Diabetics

Key Takeaways
- High morning blood sugar in non-diabetics: Fasting morning glucose levels should ideally stay between 70-90 mg/dL for optimal metabolic health.
- Dawn phenomenon: A natural hormone surge in the early morning signals your liver to release glucose, providing energy to help you wake up.
- Managing morning spikes: Adjusting your evening meal to focus on protein and fiber, and walking after dinner, can stabilize overnight and morning fasting levels.
- High morning blood sugar in non-diabetics: Fasting morning glucose levels should ideally stay between 70-90 mg/dL for optimal metabolic health.
- Dawn phenomenon: A natural hormone surge in the early morning signals your liver to release glucose, providing energy to help you wake up.
- Managing morning spikes: Adjusting your evening meal to focus on protein and fiber, and walking after dinner, can stabilize overnight and morning fasting levels.
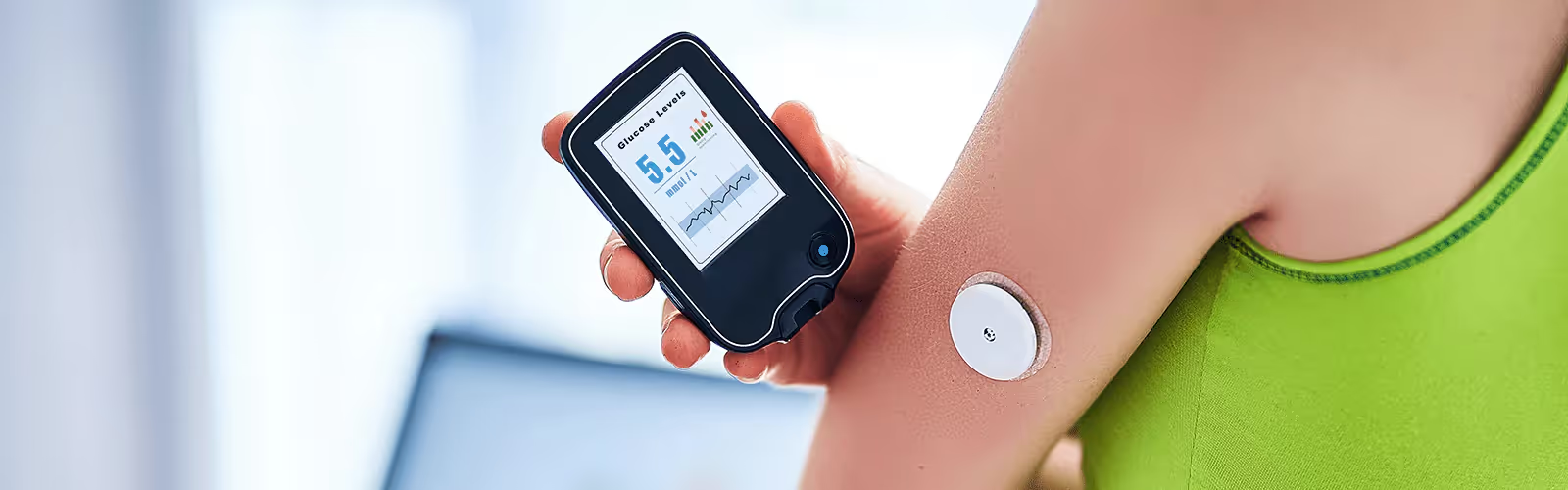
For a non-diabetic individual, glucose levels around 3 AM should be in a stable and lower range, ideally between 70-90 mg/dL. This period often represents a baseline before the body naturally releases hormones that increase glucose to help you wake up, a process known as the dawn phenomenon.
Overview:
- Your glucose level around 3 AM can help determine if a morning rise is from the natural dawn phenomenon or other factors, like a late meal.
- Learn how to manage morning glucose by adjusting your evening meal's timing and composition and incorporating post-dinner activity.
- The Nutrisense program allows you to monitor glucose patterns 24/7 with a biosensor that measures glucose in interstitial fluid, helping you connect daily habits to your body's response.
There are a lot of articles online that explain why high morning glucose levels occur and what to do about them if you are diabetic or insulin-dependent. But if you are non-diabetic, you might be wondering: “How relevant are those recommendations for me?”
What should 3 AM glucose be?
For example, many in the diabetic/insulin-dependent community are (rightfully) excited if their levels get below 120 mg/dL upon waking. Mainstream recommendations are slightly more conservative and suggest a morning glucose level below 100 is normal.
But studies have shown that levels above 90 mg/dL are correlated with adverse outcomes in otherwise healthy, non-diabetic populations. Research papers have consistently shown that morning glucose levels even between 95-99 mg/dL are predictive of increased cardiovascular death, increased incidence of diabetes, and elevated cardiovascular disease (CVD) risk.
Target range non-diabetic
This is why we recommend our non-diabetic customers target a morning glucose level between 70-90 mg/dL.
If your morning glucose level is higher than you would like, then there are several strategies to lower it. But first, let’s look at why it is high in the first place. After all, as the cartoon G.I. Joe used to always say, “Knowing is half the battle.”
When a "Good" Night's Sleep Feels Off
You wake up suddenly, and the clock reads 3:15 AM. Even though you tried to do everything right with your meals and routine yesterday, you feel restless and a bit on edge. You lie awake, wondering what’s happening inside your body that can leave you feeling drained instead of rested by morning.
Why is my glucose high in the morning?
By analogy, if the temperature gauge in your car indicated the engine was running too hot, how concerned should you be? It would depend on why the engine was too hot, wouldn’t it?
If you simply forgot to get an oil change, then the fix might be quite simple. Conversely, if the problem is stemming from a glitch in one of the onboard computers and is affecting multiple systems, then you need to get to a mechanic ASAP.
Similarly, there are several known reasons for your metabolic engine to “run too hot”. Here are some of the more common ones:
What You Ate The Night Before
There is research suggesting that a high-fat, high-calorie meal (especially in men) can cause increased liver glucose production and temporarily elevated fasting glucose levels. The increase in free fatty acids from that meal can impair insulin sensitivity and increase glucose production. This effect is especially pronounced if you combine high fat + high carbohydrate + high calorie, which is a common formula found in foods such as pizza, ice cream, fried food, etc.

In fact, the high-fat + high-carb + high-calorie phenomenon is something we consistently see in the CGM data from our users. Our Director of Nutrition, Kara Collier, made this observation while on the Fundamental Health podcast:
“A refined carbohydrate plus a refined oil, this is every snack food that has ever existed...and this food, when you have the combination of refined carbohydrate and refined oil, it creates a huge area under the curve. The fat slows down digestion, but you still have the refined carbohydrate in your system, so your body is processing it for a long time...[T]hese sort of meals lead to a massive area under the curve because your body is processing this huge load of carbohydrates/glucose, and it’s stressful on the cell and the mitochondria.”
When Kara refers to the “area under the curve”, she is referring to the amount of time that your body is in a state of high glucose.
When you consume a meal that is high in the “Trifecta” (high-fat + high-carb + high-calorie) late at night, your glucose readings will be elevated into the morning. Instead of quickly clearing the glucose, your body spends hours and hours in a high-glucose state, which sets you up for high readings in the morning.
When You Ate The Night Before
In addition to what you eat, you also need to consider when you eat.
Eating late into the night can cause your morning glucose values to be high. Your cells are not as sensitive to insulin later at night, which can cause a higher and more prolonged glucose response to meals eaten late.
A recent randomized controlled trial in adults with metabolic syndrome found that shifting to a personalized 8–10 hour eating window modestly improved glycemic regulation (HbA1c −0.10%) compared with standard counseling alone. In plain terms, compressing meals earlier in the day can support steadier glucose patterns without changing total calories.
Conversely, another study found that consuming more than 45% of daily calories after 5 p.m. was associated with higher glucose levels and less favorable metabolic patterns, even after accounting for weight and body fat.
High Stress Levels
The phrase “don’t be so stressed” can feel like a bit of a cliché. But like most clichés, it contains a significant kernel of truth.
The underlying physiological response to stress goes back over 500 million years. The stress response appears to have evolved because it provided a survival advantage in situations that were life-or-death. If your body needs energy right now to escape a threat, then relying on your digestive system is insufficient. You need a system that will liberate energy stores immediately.

Fortunately, that is exactly what your body’s stress response does. When your body senses a stressful situation, it causes a release of hormones like cortisol and adrenaline that tell the body: “Produce energy NOW.” Part of this signal stimulates the liver to create and release new glucose into the bloodstream so that energy is readily available to fuel muscular activity.
In the context of an ancestral environment, this system works great. The problem, however, is that chronic stress can cause this response to occur at low levels all the time. When that occurs, it can cause your glucose values to rise even if you have not eaten, as happens in the case of sleep.
If you want to learn more about the role of stress and how to combat it, you can find additional strategies and resources in our article on managing stress and biohacking the cortisol response.
Poor Night of Sleep
A poor night of sleep (both disrupted sleep and shortened sleep) can cause your body to be in a state of insulin resistance the next day. Insulin resistance means the cells of your body are less sensitive to the signal from insulin.
Since insulin is one of the main mechanisms by which your body manages glucose levels, this can lead to higher fasting glucose values and higher glucose responses to meals.
Surprisingly, even a single night of poor sleep can increase insulin resistance the following day. Compound that day-in and day-out, and the stage is set for chronically high glucose levels.
Lack of Physical Exercise
Exercise is a powerful tool for controlling glucose levels. There are multiple mechanisms by which exercise positively impacts glucose levels, including:
- Increased glucose uptake through non-insulin-mediated glucose uptake
- Improved insulin sensitivity independent of weight loss
- Increased glucose storage space through increased muscle glycogen stores
But perhaps the most important aspect of exercise is consistency. In adults with type 2 diabetes, consistent physical activity supports better insulin sensitivity, with benefits that can persist beyond 72 hours post-workout. Using a CGM for fitness insights may be a helpful tool to help you make sure you are optimally fueling your body for exercise.
Metabolic Syndrome
Elevated fasting glucose values could be a sign of a temporary problem, like we discussed with a lack of sleep. However, they can also be a sign of a bigger problem, like metabolic syndrome.
In addition to fasting glucose levels, there are 4 other risk factors involved in metabolic syndrome: triglycerides, HDL, blood pressure, and waist circumference. If your markers are outside the recommended ranges for these risk factors, then you may want to consult with a qualified professional.
Dawn Phenomenon
The dawn phenomenon is a natural occurrence that happens in all people. In the early morning hours, between 3 AM and 8 AM, certain hormones, such as growth hormone, cortisol, and catecholamines, cause the liver to release extra glucose. This signal acts like your body’s natural “alarm clock” and gives your body access to easily available energy to get moving.
Some people seem more sensitive to this effect and have slightly higher glucose values upon waking that can exceed 100 mg/dL, but about 1 hour after waking they are back down to normal, optimal levels.
3 AM Check - Dawn Pattern or Rebound High
A quick 3 AM check can help you pinpoint why your morning glucose is elevated. A steady rise from about 3 to 8 AM without an overnight low is consistent with a dawn pattern, while a low around 3 AM followed by a higher value on waking can indicate a rebound hyperglycemia pattern sometimes called the Somogyi effect.
If you use a continuous glucose monitor, remember it reports glucose measured in interstitial fluid. Professional guidance supports using CGM traces and targeted overnight checks to evaluate nocturnal patterns, hypoglycemia, and Time in Range. See the ADA Diabetes Technology standards for details.
How to try this across 2 to 3 nights
- Log dinner timing and composition, activity, stress, and your 3 AM reading in the Nutrisense app.
- Compare patterns the next morning: gradual rise without a low versus a low at 3 AM with a higher waking reading.
- If you notice overnight lows or symptoms such as sweating, shaking, restless sleep, nightmares, morning headache, or confusion, contact your clinician and follow their guidance for treating hypoglycemia. Hypoglycemia unawareness can blunt symptoms during sleep, and CGM review can help detect nocturnal lows. See ADA Glycemic Goals and Hypoglycemia.
Make Time in Range part of your check-in
Time in Range (TIR) is the percentage of time your readings fall within your chosen target range, and it gives you a simple way to compare nights as you test one change at a time. TIR is a core CGM metric in the ADA Diabetes Technology standards.
Recheck after waking
With Nutrisense, you can use a CGM without diabetes to monitor your glucose levels one to two hours after waking to see if they have naturally lowered on their own.
How to prevent high morning glucose
We have explored why your morning glucose level might be high. Now, let’s explore how we can take action to address it.
Our team has analyzed non-diabetic glucose monitoring data from our users, and found that there are several strategies that consistently improve morning glucose levels. The ones that tend to produce the biggest ROI include:
Prioritize Protein and Non-Starchy Vegetables at Dinner
Remember how we talked about the “Trifecta” of glucose-raising badness: high-fat + high-carb + high-calorie? If we knock out one or more of the “legs” of the Trifecta stool, then we can mitigate its adverse effects.
Based on our data, we recommend knocking out the “high-carb” leg and the “high-calorie” leg. Focusing your evening meal around full-fat protein and fiber (as tolerated) helps to create a meal that results in stable glucose levels throughout the night and into the morning.
This could look like:
- Grass-fed steak + asparagus
- Wild-caught salmon + lemon/mushrooms/tomatoes/avocados
- Pasture-raised chicken + baked veggies (zucchini, cucumber, broccoli, etc.)
- Organ stir fry (liver, kidney, heart) + Brussels sprouts/garlic/onions
Of course, individual response to food varies, but this food pattern tends to work very well for most people.
Avoid Food at Least 3 Hours Before Bed
Food too close to bedtime causes us to metabolize food poorly while we are sleeping, which can lead to higher glucose values the next morning. Eating earlier, however, allows you to take advantage of higher insulin sensitivity and gives adequate time for the parasympathetic nervous system to begin the process of digestion.

The remedy is simple: try to finish eating all food for the day at least 3 hours before you go to bed. Ideally, this would also include beverages that contain non-caloric sweeteners since they appear to have metabolic effects in the body.
Monitor Stress Levels
When we are in a fasted state, most of the glucose in circulation is coming from the liver. Hormones like cortisol send a direct message to the liver to release more energy (glucose). Since cortisol is preferentially stimulated as part of the stress response, managing stress levels is key to stable morning glucose values.
What counts as “stress” is highly variable from person to person, as are the strategies for mitigating it. Some of the tried-and-true stress management techniques include:
- Social interaction (preferably face-to-face) with a close friend or loved one
- Light physical movement (going for a walk, light gardening, playing with your kids)
- Journaling
- Prayer or gratitude
- Meditation & mindfulness
- Spending time in nature
- Periods of “device detox” (turn them off!)
- Periods of social media “detox”
- Warm bath or sauna before bed
Get Adequate Quantity and Quality of Sleep
Your mom was right - sleep is important. Sleep is a bit of a Catch-22. Both the quantity and quality of sleep are affected by glucose levels, yet glucose levels are also modulated by sleep.
So, where do you start?
You can always begin with the fundamentals of sleep hygiene:
- Make sleep a priority (as if you are setting an appointment with an important client)
- Cool, dark, quiet environment
- Consistent sleep schedule (yes, adults need bedtimes too!)
- Monitor caffeine intake, particularly within 10-12 hours of sleep
- Adequate early morning light exposure
- Restricted light & screen exposure within 2-3 hours of sleep
Additionally, rather than thinking of sleep as an isolated tool, think of it as a synergistic link. Like a chain of people connected together, each link supports the other.
If your sleep consistency and quality are inadequate, sometimes strengthening the other “links” can indirectly improve them. We’ve already discussed some of these links: nutrition, exercise, and stress management.
Keep a Consistent Exercise Routine
The best exercise is the one you do regularly. Don’t let the “perfect” become the enemy of “good enough”. It is far better to consistently walk 15 minutes a day or strength train three times per week than it is to grind out a marathon-like workout once every 3 or 4 months when the motivation strikes.
Find a movement practice that you love doing (or that you can learn to love!) and make it a non-negotiable part of your life. Leverage the insights from behavioral science to design your environment for success.
What if my glucose is low in the morning?
Low glucose in the mornings is much less common for a non-diabetic than high glucose levels. We have many counter-regulatory processes in place to make sure our glucose never goes low, since low glucose can be very dangerous.
The body has a wide arsenal of tools at its disposal for managing low glucose states including insulin, glucagon, norepinephrine, growth hormone, cortisol, and more.
All that being said, if you are experiencing low glucose in the morning here are a few things to consider:
Alcohol Intake
It is well known in the diabetic community that alcohol consumption can increase hypoglycemic events. In those who are insulin-dependent, these hypoglycemic events can even be fatal.
Alcohol is technically a toxin in the human body, and the organ responsible for alcohol detoxification is the liver. Unfortunately, the detoxification process impairs the liver’s ability to release glucose into the bloodstream. As a result, you can end up with low glucose levels in the blood.
Try Changing your Exercise Timing

Your body only has two major storage pools for glucose: the muscles and the liver. Late evening exercise - particularly if it is long in duration or high-intensity - can significantly deplete those stores. Combined with inadequate re-fueling, some people can experience hypoglycemia the following morning.
History of Bariatric Surgery or Altered Digestive Tract
Interestingly, research indicates that operations like Roux-en-Y gastric bypass can potentially cause hypoglycemia while fasted.
Adrenal Insufficiency
While rare, research has found that hypoglycemia can be a result of adrenal insufficiency in a subset of patients.
Eating Disorders or Malnutrition
Malnutrition, particularly in the setting of high body fat and muscle depletion, can also cause hypoglycemia due to limited substrates for gluconeogenesis and glycogenolysis.
How can you prevent low morning glucose?
Morning lows often start with what happened yesterday. Alcohol, evening workouts, long breaks between meals, or not enough calories are common triggers. Make one small change and see how your next-morning glucose responds.
Monitor Your Alcohol Intake
According to the Centers for Disease Control and Prevention, drinking is considered to be in the moderate or low-risk range for women at one drink or less in a day and no more than 7 drinks per week. For men, it is two drinks or less in a day and no more than 14 drinks per week.
If you still find your glucose levels are low, try cutting the NIAAA’s recommendation in half (3-4 drinks per week for women and 7 drinks per week for men).
Switch Up Your Exercise Timing
As previously discussed, exercise done too close to bed can result in hypoglycemia. If you tend to exercise in the evening, try exercising in the morning or at lunch and see if it makes a difference in your morning glucose level.
If you are particularly stretched for time, you can also try splitting up your exercise into two smaller time-blocks. This has the added advantage of giving your body more time to recover.
Get Adequate Nutrition Throughout The Day
If you are restricting calories to lose weight, your body may not be getting enough of the basic building blocks it needs to properly manage glucose levels. The same thing can happen in those who are very physically active and consuming energy-dense, but nutrient-poor, diets.
How the body’s fuel systems interact
While it is beyond the scope of this article, there is a dynamic interplay between the various metabolic pathways of the body: fat metabolism, ketone metabolism, glucose metabolism, protein metabolism, and more. Your glucose needs can significantly vary depending on which of these metabolic pathways are dominant.
The liver holds approximately 100g of glucose in the form of glycogen. It takes about 24 hours for it to be depleted while fasting or ~90 minutes of moderate-high intensity. Glucose can be synthesized from several substrates (fatty acids, lactate, amino acids, etc.), but generally speaking, it is easiest to simply consume the glucose you need.
Dialing in daily carbohydrates
A relatively sedentary person may do well with 50-100g of carbohydrates per day, whereas an athlete or a person with a physically demanding job may do best with 2-4 times that value. The best way to determine your needs, of course, is through accurate monitoring of your glucose levels.
Read your morning curve
Troubleshooting morning glucose levels can be tricky. As we have discussed, there are a lot of factors that influence overall glucose status in the body. Exercise, stress, circadian rhythm, macronutrient composition, nutrient timing, and more are continually affecting glucose management in your body.

If your morning glucose levels are higher (or lower) than you would like, always start by considering the four fundamentals and determine how you can optimize these areas for better overall wellness:
- Sleep
- Nutrition
- Exercise
- Stress management
Find the right Nutrisense programto turn insight into progress.
Frequently Asked Questions
Why does my blood sugar spike when I wake up?
Morning blood sugar spikes are typically caused by the dawn phenomenon or a late-night meal that hasn’t fully processed. In non-diabetics, this rise is a normal physiological response to hormones like cortisol that naturally increase before waking.
Are glucose levels higher in the morning?
Yes, it is common for glucose levels to be slightly higher in the early morning than during the middle of the night. This natural elevation is driven by the body releasing stored energy to help you wake up and start the day.
What should blood sugar be at bedtime without diabetes?
For individuals without diabetes, blood sugar should ideally return to baseline levels before bedtime, generally below 100 mg/dL. Finishing your last meal at least three hours before sleeping gives your metabolism time to process glucose before resting.
Go Beyond Glucose Data with Nutrisense
Your glucose can significantly impact how your body feels and functions. That’s why stable levels are an important factor in supporting overall wellbeing. But viewing glucose isn't enough. Nutrisense, you’ll be able to learn how to use your body's data to make informed lifestyle choices that support healthy living.
One-to-one coaching
Sign up to access insurance-covered video calls to work with a glucose expert: a personal registered dietitian or certified nutritionist who will help tailor your lifestyle and diet to your goals.
Monitor and measure what matters
With the Nutrisense CGM Program, you can monitor your glucose with health tech like glucose biosensors and continuous glucose monitor (CGM)s, and analyze the trends over time with the Nutrisense App. This will help you make the most informed choices about the foods you consume and their impact on your health.
Find your best fit
Ready to take the first step? Start with our quiz to find the right Nutrisense program to help you take control.
Go Beyond Glucose Data with Nutrisense
Your glucose can significantly impact how your body feels and functions. That’s why stable levels are an important factor in supporting overall wellbeing. But viewing glucose isn't enough. With Nutrisense, you’ll be able to learn how to use your body's data to make informed lifestyle choices that support healthy living.
Dietitian guidance
Sign up to access insurance-covered video calls with a glucose expert: a personal registered dietitian or certified nutritionist who will help tailor your lifestyle and diet to your goals.
Nutrisense program and app
With the Nutrisense program, you can monitor your glucose with health tech like glucose biosensors and continuous glucose monitors (CGMs), and analyze the trends over time with the Nutrisense App. This will help you make the most informed choices about the foods you consume and their impact on your health.
Get started
Ready to take the first step? Start with our quiz to find the right Nutrisense program to help you take control.

Jordyn has a bachelor’s degree in biology, a graduate degree in Human Nutrition and completed a dietetic internship at the Memphis VA. She's a dietitian at Nutrisense, and has experience working as a clinical dietitian at a VA medical center specializing in oncology and at the Mayo Clinic, working with a wide range of patients ranging from neonates in the NICU to adult ICU.