Glucose Levels Won’t Go Down? Here’s 14 Reasons Why

Key Takeaways
- Persistent high glucose: Glucose can stay elevated due to dehydration, late meals, high-carb high-fat foods, stress, illness, poor sleep, hormones, and insulin resistance.
- High glucose without eating: Even when fasting, stress hormones and dehydration can trigger the liver to release stored glucose into the bloodstream.
- Medication factors: Glucose may stay high if insulin or other medications no longer match current needs, especially during illness or steroid use.
- Persistent high glucose: Glucose can stay elevated due to dehydration, late meals, high-carb high-fat foods, stress, illness, poor sleep, hormones, and insulin resistance.
- High glucose without eating: Even when fasting, stress hormones and dehydration can trigger the liver to release stored glucose into the bloodstream.
- Medication factors: Glucose may stay high if insulin or other medications no longer match current needs, especially during illness or steroid use.
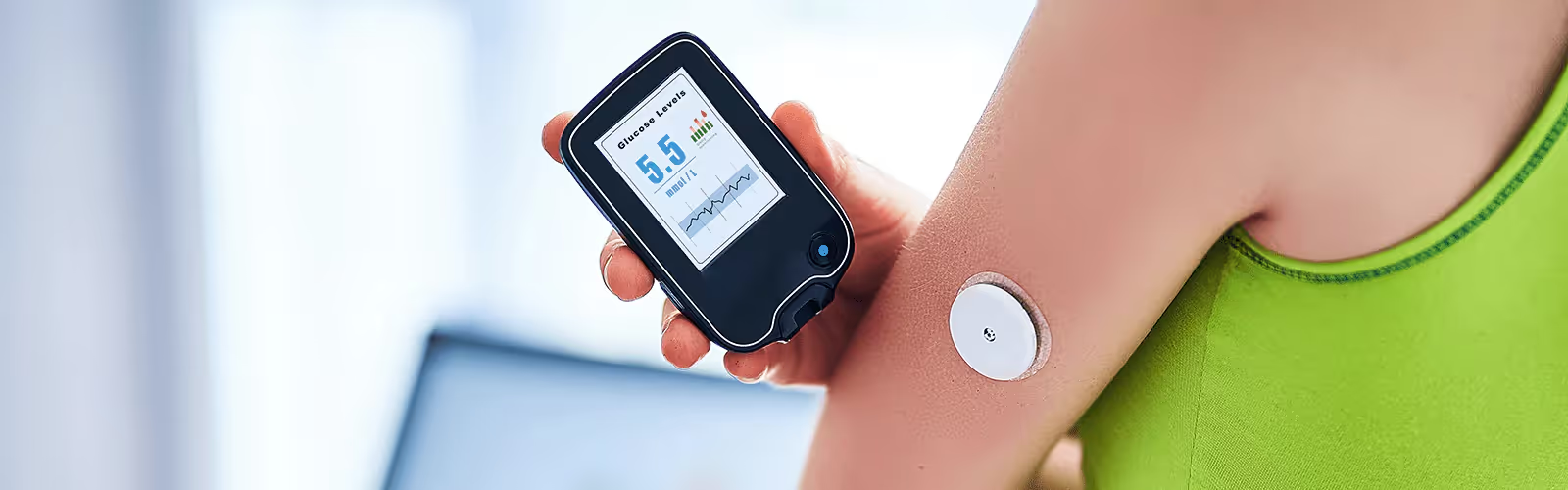
Glucose is an essential source of energy for human life. Both simple and complex sugars are broken down into glucose by the digestive system for our cells to use. Once in the blood, glucose is taken into cells by insulin, a hormone produced by the pancreas and used throughout the body.
Consuming sugary foods is the most direct method to induce a glucose spike, but intense exercise also has the same effect. During intense exercise, the body uses stored glucose, called glycogen, for fuel.
In both cases, the short rise in blood sugar within a healthy range is a sign your body is functioning normally and handling glucose in a way that sweeps it out of your blood when you don't need it and back in when you do. However, if blood sugar spikes occur too often, it may be a sign that something has gone awry with how your body handles glucose.
One of the most common reasons for long-term high blood glucose levels is diabetes mellitus, in which the body has lost the ability to produce or respond to insulin and glucose remains elevated in the blood. For people with diabetes, blood sugar spikes are a common problem when their diabetes medication wears off, when they don't have a meal plan that works for them, or when they are not within a healthy weight, causing their bodies to be less sensitive to insulin.
For people who don't have diabetes, certain medical conditions, such as obesity, heart disease and kidney disease, are known to affect insulin production and cause blood glucose fluctuations. Additionally, a sedentary lifestyle and poor eating habits also contribute to frequent blood sugar spikes.
Other common causes of an increase in blood sugar include chronic stress and certain dietary habits. Other times, it depends on how someone responds to their unique mix of foods and drinks, exercise patterns, and environmental factors. Here then is a short list of reasons, aside from diabetes mellitus, for chronically elevated blood sugar levels:
14 Reasons Your Blood Glucose Levels Won’t Go Down
1) Dehydration
A severe lack of water intake triggers an increased concentration of blood sugar since the total amount of water in the body is reduced. This means that the blood becomes more concentrated, causing an increase in blood glucose levels.
For both diabetic and non-diabetic individuals who engage in strenuous physical activity or regular exercise, particularly in hot weather, hydration is key to preventing hyperglycemia and diabetic ketoacidosis.
2) Eating Late at Night
Our bodies process food and carbohydrates best during daylight hours. When we have large food intakes later in the evening, especially those with a high sugar content, it usually triggers big swings in blood sugar levels and disrupts our sleep quality. In some cases, the glucose elevations persist into the morning, depending on the metabolism of the individual.
3) Large Meals High in Both Carbohydrates and Fat
Eating a large meal that is high in both carbohydrates and fats often causes a prolonged elevation in blood glucose. While carbs are a major contributor to blood glucose levels, fat also plays a role in increasing the duration of these elevations. Because high-fat meals slow down digestion and the absorption of carbohydrates, it results in a delayed release of sugar into the bloodstream.
Meals high in carbohydrates and fat include things like fried foods, cheesy pasta, pizza, etc. The fat in the meal slows down the digestion and absorption of the glucose, causing the glucose to slowly be processed over a long period of time.
4) Obesity

As an independent risk factor for developing type 2 diabetes, obesity contributes to insulin resistance, causing the pancreas to overwork, shuttling glucose from the blood into cells. One possible explanation for this phenomenon is that fat cells, also known as adipocytes, release fatty acids into the bloodstream, leading to a decrease in glucose uptake by cells.
Another potential reason is that overfilled adipocytes (fat cells) cause mild chronic inflammation that interferes with the insulin signaling pathway, resulting in insulin resistance. With obesity being a significant risk factor for diabetes, it is essential to maintain a healthy weight through diet and exercise to reduce your chances of developing type 2 diabetes.
5) Sedentary Lifestyle

No matter if it is low to moderate exercise routines, exercise at any level and duration has a positive impact on insulin sensitivity. Using muscle cells for cardio or weight training leads to increased glucose uptake by those muscles, which use it as fuel. The resulting risk of diabetes is reduced by over half when exercise is combined with moderate weight loss.
6) Stress
The stress hormone cortisol can lead to increased blood glucose levels. This is an essential part of the "fight or flight" response. In human evolution, this response assisted in the ability to quickly respond to potential threats or dangers. Short-term stressors, such as discovering a predator or other threat, lead to increased demands for glucose as the body needs to run or engage in combat.
Today, these stressors are usually related to work or home life. Unfortunately, modern world stressors are not acute but rather are chronic. This causes our glucose levels and blood pressure to be persistently elevated and increases the risk of developing type 2 diabetes.
7) Steroids
In some cases, people are prescribed steroids like dexamethasone or cortisone that have similar effects as the naturally-produced steroid hormone cortisol. For this reason, such prescriptions are often short-term to avoid the consequences of chronic stress, but in rarer cases, longer prescriptions are needed.
8) Eating Habits

For better or worse, one popular eating habit is known as "grazing," in which someone eats small amounts of food throughout the day. Although it may sound healthy since it avoids big meals, grazing results in overall higher calorie consumption, which eventually leads to weight gain and higher blood glucose levels. At the same time, constant snacking triggers a constant release of insulin, leading to insulin resistance and increasing the risk of type 2 diabetes.
9) Endocrinopathies
The endocrine system is closely related to the blood glucose regulation process. When the endocrine system isn't functioning properly, it results in hormonal imbalances that trigger long-term high blood glucose levels. Common endocrine disorders (other than diabetes mellitus) that cause persistently high levels of cortisol or glucagon are Cushing's Syndrome, acromegaly, and hyperthyroidism.
10) Non-Endocrine Illness
Common illnesses, such as when we have a cold or the flu, often result in consistently increased glucose readings. When we have a cold or flu, our body deploys many different hormones which heighten our immune response to fight off the cold.
It is similar to our stress response, and an unfortunate downside is that this shift in hormones causes us to make more glucose and to be slightly less sensitive to the effects of insulin.
11) Sleeplessness

Any disruption to the circadian cycle increases insulin resistance. Imagine what graveyard shift workers, people with sleep apnea, and insomniacs go through. In general, seven to nine hours of sleep per night is recommended for adults.
Additionally, individuals who experience fatigue due to poor sleep quality are more likely to develop type 2 diabetes. One of the most common reasons is due to constant waking because of obstructive sleep apnea. (OSA). OSA causes pauses in breathing during sleep, leading to decreased oxygen levels. When the brain senses the decrease in oxygen, it releases stress cortisol hormones that raise blood sugar levels and increase insulin resistance.
12) Alcohol
While drinking alcohol (ethanol), there's a short-term decrease in blood glucose levels followed by an increase in blood glucose lasting hours to days. This may be due to a change in insulin and glucagon balances or because the liver prioritizes metabolizing alcohol which is technically a toxin (hence "intoxicated"), over the normal process of storing glucose as glycogen.
13) Female Hormones
The insulin level and insulin resistance in women are closely linked to their monthly hormone cycle. As estrogen levels drop during a woman's luteal phase and menopause, it causes an increase in insulin resistance. Other common symptoms include weight gain, difficulty losing weight, and fatigue. Studies show that estrogen replacement therapy helps improve insulin sensitivity and glucose tolerance in postmenopausal women.
14) Gut Microflora
The digestive tract contains billions of bacteria, fungi, and other microorganisms that play a vital role in our health. This collection of microorganisms is known as the gut microflora. Studies have found a link between imbalances in gut bacteria and insulin resistance in both humans and animals.
Certain types of bacteria affect insulin sensitivity, inflammation levels, and even the production of hormones related to hunger and satiety. A healthy gut microflora has been associated with better blood sugar control and a decreased risk of developing Type 2 diabetes. When the good bacteria are out of equilibrium, the flourishing bad bacteria reduce insulin secretion, release fatty acids, and cause adipocyte inflammation.
Engage with Your Blood Glucose Levels with Nutrisense
Your blood sugar levels have a profound impact on how your body feels and functions. That's why maintaining stable blood glucose levels is crucial for supporting your overall well-being.
With Nutrisense, you can easily track your blood glucose levels over time using a continuous glucose monitor (CGM). This technology allows you to see real-time data and trends of your blood sugar levels, giving you insights into how your body responds to different foods, stressors, and other lifestyle factors.
But Nutrisense is more than just a tracking tool. When you become part of the Nutrisense CGM program, our team of trusted nutritionists is here to provide you with additional support and guidance. We understand that everyone's journey is unique, and we're here to help you achieve your goals.
Are you ready to take the first step? Start by taking our quiz to discover how Nutrisense can support your health and well-being. You deserve to live your best life, and we're here to support you every step of the way.
Find the right Nutrisense programto turn insight into progress.
Frequently Asked Questions
Why is my blood sugar not going down with insulin?
Glucose can stay high with insulin when the dose no longer matches your current metabolic needs. Illness, stress, steroid use, and increased insulin resistance can make it harder for medication to bring levels down. A clinician can help review your regimen.
How long does it take for high blood sugar to go down?
It depends on the underlying driver and your individual metabolism. While a meal-related spike may resolve in a few hours, elevations driven by illness, chronic stress, or hormones can take much longer to stabilize.
Will blood sugar go up if you don't eat?
Yes. Fasting, skipping meals, and dehydration can trigger stress hormones that prompt your liver to release stored glucose. This is why levels can rise even without food intake.
Go Beyond Glucose Data with Nutrisense
Your glucose can significantly impact how your body feels and functions. That’s why stable levels are an important factor in supporting overall wellbeing. But viewing glucose isn't enough. Nutrisense, you’ll be able to learn how to use your body's data to make informed lifestyle choices that support healthy living.
One-to-one coaching
Sign up to access insurance-covered video calls to work with a glucose expert: a personal registered dietitian or certified nutritionist who will help tailor your lifestyle and diet to your goals.
Monitor and measure what matters
With the Nutrisense CGM Program, you can monitor your glucose with health tech like glucose biosensors and continuous glucose monitor (CGM)s, and analyze the trends over time with the Nutrisense App. This will help you make the most informed choices about the foods you consume and their impact on your health.
Find your best fit
Ready to take the first step? Start with our quiz to find the right Nutrisense program to help you take control.

Kara Collier is a registered dietitian nutritionist and certified nutrition support clinician who is passionate about reshaping how we approach prevention, behavior change, and metabolic health. A Forbes 30 Under 30 honoree, she’s helped over 150,000 people improve their metabolic health using tools like continuous glucose monitors and behavior-focused nutrition strategies. Kara has been featured by Forbes, UC Berkeley, and HLTH, and has appeared on top podcasts like Mind Pump and The Genius Life.